Social Work Practice with Carers


Case Study 2: Josef
Download the whole case study as a PDF file
Josef is 16 and lives with his mother, Dorota, who was diagnosed with Bipolar disorder seven years ago. Josef was born in England. His parents are Polish and his father sees him infrequently.
This case study looks at the impact of caring for someone with a mental health problem and of being a young carer , in particular the impact on education and future employment .
When you have looked at the materials for the case study and considered these topics, you can use the critical reflection tool and the action planning tool to consider your own practice.
- One-page profile
Support plan
Transcript (.pdf, 48KB)
Name : Josef Mazur
Gender : Male
Ethnicity : White European
Download resource as a PDF file
First language : English/ Polish
Religion : Roman Catholic
Josef lives in a small town with his mother Dorota who is 39. Dorota was diagnosed with Bi-polar disorder seven years ago after she was admitted to hospital. She is currently unable to work. Josef’s father, Stefan, lives in the same town and he sees him every few weeks. Josef was born in England. His parents are Polish and he speaks Polish at home.
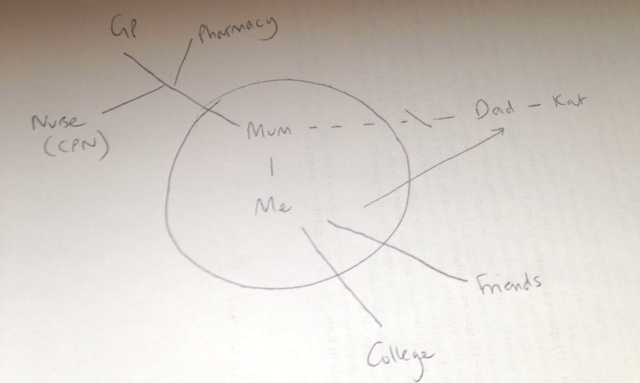
Josef is doing a foundation art course at college. Dorota is quite isolated because she often finds it difficult to leave the house. Dorota takes medication and had regular visits from the Community Psychiatric Nurse when she was diagnosed and support from the Community Mental Health team to sort out her finances. Josef does the shopping and collects prescriptions. He also helps with letters and forms because Dorota doesn’t understand all the English. Dorota gets worried when Josef is out. When Dorota is feeling depressed, Josef stays at home with her. When Dorota is heading for a high, she tries to take Josef to do ‘exciting stuff’ as she calls it. She also spends a lot of money and is very restless.
Josef worries about his mother’s moods. He is worried about her not being happy and concerned at the money she spends when she is in a high mood state. Josef struggles to manage his day around his mother’s demands and to sleep when she is high. Josef has not told anyone about the support he gives to his mother. He is embarrassed by some of the things she does and is teased by his friends, and he does not think of himself as a carer. Josef has recently had trouble keeping up with course work and attendance. He has been invited to a meeting with his tutor to formally review attendance and is worried he will get kicked out. Josef has some friends but he doesn’t have anyone he can confide in. His father doesn’t speak to his mother.
Josef sees some information on line about having a parent with a mental health problem. He sends a contact form to ask for information. Someone rings him and he agrees to come into the young carers’ team and talk to the social worker. You have completed the assessment form with Josef in his words and then done a support plan with him.
Back to Summary
Josef Mazur
What others like and admire about me
Good at football
Finished Arkham Asylum on expert level
What is important to me
Mum being well and happy
Seeing my dad
Being an artist
Seeing my friends
How best to support me
Tell me how to help mum better
Don’t talk down to me
Talk to me 1 to 1
Let me know who to contact if I am worried about something
Work out how I can have some time on my own so I can do my college work and see my friends
Don’t tell mum and my friends
Date chronology completed : 7 March 2016
Date chronology shared with person: 7 March 2016
| 1997 | Josef’s mother and father moved to England from Poznan. | Both worked at the warehouse – Father still works there. |
| 11.11.1999 | Josef born. | Mother worked for some of the time that Josef was young. |
| 2006 | Josef reports that his mother and father started arguing about this time because of money and Josef’s mother not looking after household tasks. | Josef started doing household tasks e.g. cleaning, washing and ironing. |
| 2008 | Josef reports that his mother didn’t get out of bed for a few months. | Josef managed the household during this period. |
| October 2008 | Josef reports that his mother spent lots of money in catalogues and didn’t sleep. She was admitted to hospital. | Mother was in hospital for 6 weeks and was diagnosed with bipolar disorder. Josef began looking after his mother’s medication and says that he started to ‘keep an eye on her.’ |
| May 2010 | Josef’s father moved out to live with his friend Kat. Josef stayed with his mother. | Josef reports that his mother was ‘really sad for a while and then she went round and shouted at them.’ Mother started on different medication and had regular visits from the Community Psychiatric Nurse. Josef said that the CPN told him about his mum’s illness and to let him know if he needed any help but he was managing ok. Josef saw his father every week for a few years and then it was more like every month. Father does not visit Josef or speak to his mother. |
| 2013/14 | Josef reports that his mother got into a lot of debt and they had eviction letters. | Josef’s father paid some of the bills and his mother was referred by the Community Mental Health Team for advice from CAB and started getting benefits. Josef started doing the correspondence. |
| 2015 | Josef left school and went to college. | Josef got an A (art), 4 Cs and 3 Ds GCSE. He says that he ‘would have done better but I didn’t do much work.’ |
| 26 Feb 2016 | Josef got a letter from his tutor at college saying he had to go to a formal review about attendance. | Josef saw information on-line about having a parent with a mental health problem and asked for some information. |
| 2 March 2016 | Phone call from young carer’s team to Josef. | Josef agreed to come in for an assessment. |
| 4 March 2016 | Social worker meets with Josef. | Carer’s assessment and support plan completed. |
| 7 March 2016 | Paperwork completed. | Sent to Josef. |
Young Carers Assessment
Do you look after or care for someone at home?
The questions in this paper are designed to help you think about your caring role and what support you might need to make your life a little easier or help you make time for more fun stuff.
Please feel free to make notes, draw pictures or use the form however is best for you.
What will happen to this booklet?
This is your booklet and it is your way to tell an adult who you trust about your caring at home. This will help you and the adult find ways to make your life and your caring role easier.
The adult who works with you on your booklet might be able to help you with everything you need. If they can’t, they might know other people who can.
Our Agreement
- I will share this booklet with people if I think they can help you or your family
- I will let you know who I share this with, unless I am worried about your safety, about crime or cannot contact you
- Only I or someone from my team will share this booklet
- I will make sure this booklet is stored securely
- Some details from this booklet might be used for monitoring purposes, which is how we check that we are working with everyone we should be
Signed: ___________________________________
Young person:
- I know that this booklet might get shared with other people who can help me and my family so that I don’t have to explain it all over again
- I understand what my worker will do with this booklet and the information in it (written above).
Signed: ____________________________________
Name : Josef Mazur Address : 1 Green Avenue, Churchville, ZZ1 Z11 Telephone: 012345 123456 Email: [email protected] Gender : Male Date of birth : 11.11.1999 Age: 16 School : Green College, Churchville Ethnicity : White European First language : English/ Polish Religion : Baptised Roman Catholic GP : Dr Amp, Hill Surgery
The best way to get in touch with me is:
Do you need any support with communication?
*Josef is bilingual – English and Polish. He speaks English at school and with his friends, and Polish at home. Josef was happy to have this assessment in English, however, another time he may want to have a Polish interpreter. It will be important to ensure that Josef is able to use the words he feels best express himself.
About the person/ people I care for
I look after my mum who has bipolar disorder. Mum doesn’t work and doesn’t really leave the house unless she is heading for a high. When Mum is sad she just stays at home. When she is getting hyper then she wants to do exciting stuff and she spends lots of money and she doesn’t sleep.
Do you wish you knew more about their illness?
Do you live with the person you care for?
What I do as a carer It depends on if my mum has a bad day or not. When she is depressed she likes me to stay home with her and when she is getting hyper then she wants me to go out with her. If she has new meds then I like to be around. Mum doesn’t understand English very well (she is from Poland) so I do all the letters. I help out at home and help her with getting her medication.
Tell us what an average week is like for you, what kind of things do you usually do?
Monday to Friday
Get up, get breakfast, make sure mum has her pills, tell her to get up and remind her if she’s got something to do.
If mum hasn’t been to bed then encourage her to sleep a bit and set an alarm
College – keep phone on in case mum needs to call – she usually does to ask me to get something or check when I’m coming home
Go home – go to shops on the way
Remind mum about tablets, make tea and pudding for both of us as well as cleaning the house and fitting tea in-between, ironing, hoovering, hanging out and bringing in washing
Do college work when mum goes to bed if not too tired
More chores
Do proper shop
Get prescription
See my friends, do college work
Sunday – do paper round
Physical things I do….
(for example cooking, cleaning, medication, shopping, dressing, lifting, carrying, caring in the night, making doctors appointments, bathing, paying bills, caring for brothers & sisters)
I do all the housework and shopping and cooking and get medication
Things I find difficult
Emotional support I provide…. (please tell us about the things you do to support the person you care for with their feelings; this might include, reassuring them, stopping them from getting angry, looking after them if they have been drinking alcohol or taking drugs, keeping an eye on them, helping them to relax)
If mum is stressed I stay with her
If mum is depressed I have to keep things calm and try to lighten the mood
She likes me to be around
When mum is heading for a high wants to go to theme parks or book holidays and we can’t afford it
I worry that mum might end up in hospital again
Mum gets cross if I go out
Other support
Please tell us about any other support the person you care for already has in place like a doctor or nurse, or other family or friends.
The GP sees mum sometimes. She has a nurse who she can call if things get bad.
Mum’s medication comes from Morrison’s pharmacy.
Dad lives nearby but he doesn’t talk to mum.
Mum doesn’t really have any friends.
Do you ever have to stop the person you care for from trying to harm themselves or others?
Some things I need help with
Sorting out bills and having more time for myself
I would like mum to have more support and to have some friends and things to do
On a normal week, what are the best bits? What do you enjoy the most? (eg, seeing friends, playing sports, your favourite lessons at school)
Seeing friends
When mum is up and smiling
Playing football
On a normal week, what are the worst bits? What do you enjoy the least? (eg cleaning up, particular lessons at school, things you find boring or upsetting)
Nagging mum to get up
Reading letters
Missing class
Mum shouting
Friends laugh because I have to go home but they don’t have to do anything
What things do you like to do in your spare time?
Do you feel you have enough time to spend with your friends or family doing things you enjoy, most weeks?
Do you have enough time for yourself to do the things you enjoy, most weeks? (for example, spending time with friends, hobbies, sports)
Are there things that you would like to do, but can’t because of your role as a carer?
Can you say what some of these things are?
See friends after college
Go out at the weekend
Time to myself at home
It can feel a bit lonely
I’d like my mum to be like a normal mum
School/ College Do you think being your caring role makes school/college more difficult for you in any way?
If you ticked YES, please tell us what things are made difficult and what things might help you.
Things I find difficult at school/ college
Sometimes I get stressed about college and end up doing college work really late at night – I get a bit angry when I’m stressed
I don’t get all my college work done and I miss days
I am tired a lot of the time
Things I need help with…
I am really worried they will kick me out because I am behind and I miss class. I have to meet my tutor about it.
Do your teachers know about your caring role?
Are you happy for your teachers and other staff at school/college to know about your caring role?
Do you think that being a carer will make it more difficult for you to find or keep a job?
Why do you think being a carer is/ will make finding a job more difficult?
I haven’t thought about it. I don’t know if I’ll be able to finish my course and do art and then I won’t be able to be an artist.
Who will look after mum?
What would make it easier for you to find a job after school/college?
Finishing my course
Mum being ok
How I feel about life…
Do you feel confident both in school and outside of school?
Somewhere in the middle
In your life in general, how happy do you feel?
Quite unhappy
In your life in general, how safe do you feel?
How healthy do you feel at the moment?
Quite healthy
Being heard
Do you think people listen to what you are saying and how you are feeling?
If you said no, can you tell us who you feel isn’t listening or understanding you sometimes (eg, you parents, your teachers, your friends, professionals)
I haven’t told anyone
I can’t talk to mum
My friends laugh at me because I don’t go out
Do you think you are included in important decisions about you and your life? (eg, where you live, where you go to school etc)
Do you think that you’re free to make your own choices about what you do and who you spend your time with?
Not often enough
Is there anybody who knows about the caring you’re doing at the moment?
If so, who?
I told dad but he can’t do anything
Would you like someone to talk to?
Supporting me Some things that would make my life easier, help me with my caring or make me feel better
I don’t know
Fix mum’s brain
People to help me if I’m worried and they can do something about it
Not getting kicked out of college
Free time – time on my own to calm down and do work or have time to myself
Time to go out with my friends
Get some friends for mum
I don’t want my mum to get into trouble
Who can I turn to for advice or support?
I would like to be able to talk to someone without mum or friends knowing
Would you like a break from your caring role?
How easy is it to see a Doctor if you need to?
To be used by social care assessors to consider and record measures which can be taken to assist the carer with their caring role to reduce the significant impact of any needs. This should include networks of support, community services and the persons own strengths. To be eligible the carer must have significant difficulty achieving 1 or more outcomes without support; it is the assessors’ professional judgement that unless this need is met there will be a significant impact on the carer’s wellbeing. Social care funding will only be made available to meet eligible outcomes that cannot be met in any other way, i.e. social care funding is only available to meet unmet eligible needs.
Date assessment completed : 7 March 2016
Social care assessor conclusion
Josef provides daily support to his mum, Dorota, who was diagnosed with bipolar disorder seven years ago. Josef helps Dorota with managing correspondence, medication and all household tasks including shopping. When Dorota has a low mood, Josef provides support and encouragement to get up. When Dorota has a high mood, Josef helps to calm her and prevent her spending lots of money. Josef reports that Dorota has some input from community health services but there is no other support. Josef’s dad is not involved though Josef sees him sometimes, and there are no friends who can support Dorota.
Josef is a great support to his mum and is a loving son. He wants to make sure his mum is ok. However, caring for his mum is impacting: on Josef’s health because he is tired and stressed; on his emotional wellbeing as he can get angry and anxious; on his relationship with his mother and his friends; and on his education. Josef is at risk of leaving college. Josef wants to be able to support his mum better. He also needs time for himself, to develop and to relax, and to plan his future.
Eligibility decision : Eligible for support
What’s happening next : Create support plan
Completed by Name : Role : Organisation :
Name: Josef Mazur
Address 1 Green Avenue, Churchville, ZZ1 Z11
Telephone 012345 123456
Email [email protected]
Gender: Male
Date of birth: 11.11.1999 Age: 16
School Green College, Churchville
Ethnicity White European
First language English/ Polish
Religion Baptised Roman Catholic
GP Dr Amp, Hill Surgery
My relationship to this person son
Name Dorota Mazur
Gender Female
Date of birth 12.6.79 Age 36
First language Polish
Religion Roman Catholic
Support plan completed by
Organisation
|
|
| |
|
|
| |
|
| ||
|
| ||
Date of support plan: 7 March 2016
This plan will be reviewed on: 7 September 2016
Signing this form
Please ensure you read the statement below in bold, then sign and date the form.
I understand that completing this form will lead to a computer record being made which will be treated confidentially. The council will hold this information for the purpose of providing information, advice and support to meet my needs. To be able to do this the information may be shared with relevant NHS Agencies and providers of carers’ services. This will also help reduce the number of times I am asked for the same information.
If I have given details about someone else, I will make sure that they know about this.
I understand that the information I provide on this form will only be shared as allowed by the Data Protection Act.
Josef has given consent to share this support plan with the CPN but does not want it to be shared with his mum.
Mental health
The social work role with carers in adult mental health services has been described as: intervening and showing professional leadership and skill in situations characterised by high levels of social, family and interpersonal complexity, risk and ambiguity (Allen 2014). Social work with carers of people with mental health needs, is dependent on good practice with the Mental Capacity Act where practitioner knowledge and understanding has been found to be variable (Iliffe et al 2015).
- Carers Trust (2015) Mental Health Act 1983 – Revised Code of Practice Briefing
- Carers Trust (2013) The Triangle of Care Carers Included: A Guide to Best Practice in Mental Health Care in England
- Mind, Talking about mental health
- Tool 1: Triangle of care: self-assessment for mental health professionals – Carers Trust (2013) The Triangle of Care Carers Included: A Guide to Best Practice in Mental Health Care in England Second Edition (page 23 Self-assessment tool for organisations)
Mental capacity, confidentiality and consent
Social work with carers of people with mental health needs, is dependent on good practice with the Mental Capacity Act where practitioner knowledge and understanding has been found to be variable (Iliffe et al 2015). Research highlights important issues about involvement, consent and confidentiality in working with carers (RiPfA 2016, SCIE 2015, Mental Welfare Commission for Scotland 2013).
- Beddow, A., Cooper, M., Morriss, L., (2015) A CPD curriculum guide for social workers on the application of the Mental Capacity Act 2005 . Department of Health
- Bogg, D. and Chamberlain, S. (2015) Mental Capacity Act 2005 in Practice Learning Materials for Adult Social Workers . Department of Health
- Department of Health (2015) Best Interest Assessor Capabilities , The College of Social Work
- RiPfA Good Decision Making Practitioner Handbook
- SCIE Mental Capacity Act resource
- Tool 2: Making good decisions, capacity tool (page 70-71 in good decision making handbook)
Young carers
A young carer is defined as a person under 18 who provides or intends to provide care for another person. The concept of care includes practical or emotional support. It is the case that this definition excludes children providing care as part of contracted work or as voluntary work. However, the local authority can ignore this and carry out a young carer’s need assessment if they think it would be appropriate. Young carers, young adult carers and their families now have stronger rights to be identified, offered information, receive an assessment and be supported using a whole-family approach (Carers Trust 2015).
- SCIE (2015) Young carer transition in practice under the Care Act 2014
- SCIE (2015) Care Act: Transition from children’s to adult services – early and comprehensive identification
- Carers Trust (2015) Rights for young carers and young adult carers in the Children and Families Act
- Carers Trust (2015) Know your Rights: Support for Young Carers and Young Adult Carers in England
- The Children’s Society (2015) Hidden from view: The experiences of young carers in England
- DfE (2011) Improving support for young carers – family focused approaches
- ADASS and ADCS (2015) No wrong doors: working together to support young carers and their families
- Carers Trust, Supporting Young Carers and their Families: Examples of Practice
- Refugee toolkit webpage: Children and informal interpreting
- SCIE (2010) Supporting carers: the cared for person
- SCIE (2015) Care Act Transition from children’s to adults’ services – Video diaries
- Tool 3: Young carers’ rights – The Children’s Society (2014) The Know Your Rights pack for young carers in England!
- Tool 4: Vision and principles for adults’ and children’s services to work together
Young carers of parents with mental health problems
The Care Act places a duty on local authorities to assess young carers before they turn 18, so that they have the information they need to plan for their future. This is referred to as a transition assessment. Guidance, advocating a whole family approach, is available to social workers (LGA 2015, SCIE 2015, ADASS/ADCS 2011).
- SCIE (2012) At a glance 55: Think child, think parent, think family: Putting it into practice
- SCIE (2008) Research briefing 24: Experiences of children and young people caring for a parent with a mental health problem
- SCIE (2008) SCIE Research briefing 29: Black and minority ethnic parents with mental health problems and their children
- Carers Trust (2015) The Triangle of Care for Young Carers and Young Adult Carers: A Guide for Mental Health Professionals
- ADASS and ADCS (2011) Working together to improve outcomes for young carers in families affected by enduring parental mental illness or substance misuse
- Ofsted (2013) What about the children? Joint working between adult and children’s services when parents or carers have mental ill health and/or drug and alcohol problems
- Mental health foundation (2010) MyCare The challenges facing young carers of parents with a severe mental illness
- Children’s Commissioner (2012) Silent voices: supporting children and young people affected by parental alcohol misuse
- SCIE, Parental mental health and child welfare – a young person’s story
Tool 5: Family model for assessment
- Tool 6: Engaging young carers of parents with mental health problems or substance misuse
Young carers and education/ employment
Transition moments are highlighted in the research across the life course (Blythe 2010, Grant et al 2010). Complex transitions required smooth transfers, adequate support and dedicated professionals (Petch 2010). Understanding transition theory remains essential in social work practice (Crawford and Walker 2010). Partnership building expertise used by practitioners was seen as particular pertinent to transition for a young carer (Heyman 2013).
- TLAP (2013) Making it real for young carers
- Learning and Work Institute (2018) Barriers to employment for young adult carers
- Carers Trust (2014) Young Adult Carers at College and University
- Carers Trust (2013) Young Adult Carers at School: Experiences and Perceptions of Caring and Education
- Carers Trust (2014) Young Adult Carers and Employment
- Family Action (2012) BE BOTHERED! Making Education Count for Young Carers

Download The Triangle of Care as a PDF file
The Triangle of Care Carers Included: A Guide to Best Practice in Mental Health Care in England
The Triangle of Care is a therapeutic alliance between service user, staff member and carer that promotes safety, supports recovery and sustains wellbeing…

Download the Capacity Tool as a PDF file
Capacity Tool Good decision-making Practitioners’ Handbook
The Capacity tool on page 71 has been developed to take into account the lessons from research and the case CC v KK. In particular:
- that capacity assessors often do not clearly present the available options (especially those they find undesirable) to the person being assessed
- that capacity assessors often do not explore and enable a person’s own understanding and perception of the risks and advantages of different options
- that capacity assessors often do not reflect upon the extent to which their ‘protection imperative’ has influenced an assessment, which may lead them to conclude that a person’s tolerance of risks is evidence of incapacity.
The tool allows you to follow steps to ensure you support people as far as possible to make their own decisions and that you record what you have done.

Download Know your rights as a PDF file
Tool 3: Know Your Rights Young Carers in Focus
This pack aims to make you aware of your rights – your human rights, your legal rights, and your rights to access things like benefits, support and advice.
Need to know where to find things out in a hurry? Our pack has lots of links to useful and interesting resources that can help you – and help raise awareness about young carers’ issues!
Know Your Rights has been produced by Young Carers in Focus (YCiF), and funded by the Big Lottery Fund.
Tool 4: Vision and principles for adults’ and children’s services to work together to support young carers
Download the tool as a PDF file
You can use this tool to consider how well adults’ and children’s services work together, and how to improve this.

Click on the diagram to open full size in a new window
This is based on ADASS and ADCS (2015) No wrong doors : working together to support young carers and their families
Download the tool as a PDF file
You can use this tool to help you consider the whole family in an assessment or review.
What are the risk, stressors and vulnerability factors?
How is the child/ young person’s wellbeing affected?
How is the adult’s wellbeing affected?

What are the protective factors and available resources?
This tool is based on SCIE (2009) Think child, think parent, think family: a guide to parental mental health and child welfare
Tool 6: Engaging young carers
Young carers have told us these ten things are important. So we will do them.
- Introduce yourself. Tell us who you are and what your job is.
- Give us as much information as you can.
- Tell us what is wrong with our parents.
- Tell us what is going to happen next.
- Talk to us and listen to us. Remember it is not hard to speak to us we are not aliens.
- Ask us what we know and what we think. We live with our parents; we know how they have been behaving.
- Tell us it is not our fault. We can feel guilty if our mum or dad is ill. We need to know we are not to blame.
- Please don’t ignore us. Remember we are part of the family and we live there too.
- Keep on talking to us and keeping us informed. We need to know what is happening.
- Tell us if there is anyone we can talk to. Maybe it could be you.

- Equal opportunities
- Complaints procedure
- Terms and conditions
- Privacy policy
- Cookie policy
- Accessibility

Social Work Graduate
Resources for social work graduates
Various social work practice approaches
Blogs added to / updated regularly
https://www.facebook.com/socialworkgraduate
https://www.instagram.com/socialworkgraduate/
- May 5, 2022
- 19 min read
Definition, importance, information included, presentation, amending, legislation, terminating client, sharing with client, templates: SOAP, DAP, BIRP, BPSS, Intake report
Three sections follow:
1. Background Material that provides the context for the topic
2. A suggested Practice Approach
3. A list of Supporting Material / References
Feedback welcome!
Background Material

What are case notes?
Sommers-Flanagan (2009) suggest case notes reflect the information provided at an interview and usually cover the following three broad areas:
Identifying, evaluating, and exploring the client's chief complaint and associated therapy goals.
Obtaining data related to the client's interpersonal style, interpersonal skills, and personal history.
Evaluating the client's current life situation and functioning.
AASW (2016) add a fourth point: case notes should also include actions to be taken with regard to the client. Lillis (2017) elaborates: case notes could include reference to or inclusion of other documents, e.g. a care plan, a purchase order and a review summary. For Lillis, case notes are a combination of documents that successfully describe the situation, needs and actual services provided.
Why are case notes important?
Case notes have been emphasized as central to the work in which social workers engage. Case notes:
help focus work,
support effective partnerships with service users and carers,
provide a comprehensive, documented account of work with service users and their families,
assist continuity when workers change,
provide an essential tool for managers to monitor work,
can becomes a major source of evidence for investigations and enquiries.
Inadequate case records result in poor decision-making and adverse client outcomes (AASW, 2016; Lillis, 2017).
Healy and Mulholland (2007) expand many of the above points as follows. Case records are:
a vital information base for client work
formal and factual information—what the case consists of, what has been done to deal with it, when the case began, when the situation changed, the service modifications that took place, when the case ended and the final outcome
situational data on the client’s needs (phone calls, notes, emails, face-to-face interviews)
a way of clarifying the case situation for both the practice worker and the client
having the client speak, and the subsequent work presenting the case in a coherent and focused written form helps clarify the complex issues of the case for both worker and client
a means by which social workers and service users can make visible to others, such as team members, aspects of the social context of the client’s needs that might otherwise be ignored
recording case notes provides a focused social work coherence to them, frames the individuality of the client’s situation, and makes it easier for others dealing with the client to understand the situation
a method of promoting opportunities for collaborative responses in health and community services teams
a means of promoting the recognition of good practice
assist accountability, demonstrate efficiency and quality work as well as commitment and dedication
a vital information base for the achievement of consistency in social work intervention.
How and when should case notes be recorded?
Case notes can be recorded manually or electronically and should:
include on each page the name and DOB or other identifying information of the client
be recorded as soon as possible after an interaction or event
be typed or, if handwritten, clearly readable
include the name, signature and profession/role of the author
include the time of contact, particularly where there are a high volume of interactions in a day (AASW, 2016; Sommers-Flanagan, 2009).
What information should be included in a case note?
There are no prescribed rules for what we put in or out of case notes. It depends on the agency rules and our view. However they are legal documents that can be called for by the court. So in writing them consider
Who is going to read them?
How will / can the information be interpreted?
What needs to be there so someone else can go on with the case if you leave?
Put context around any judgements you make, do not just give your opinion (Maple, 2012).
Information recorded about a client should be impartial , accurate and complete with care taken to ensure that:
only details relevant to the provision of a support or service to which the client has consented are recorded
when working with involuntary clients this means recording information relevant to statutory practice
notes are free from derogatory or emotive language
subjective opinions are qualified with relevant background information, theory or research
relevant information is not omitted. (AASW, 2016)
It is important to listen for what is important to the client. Signs that a matter is important are:
Word, phrase or topic repetitions (e.g. “money” may be mentioned four times)
Use of colloquial phrases of emphasis (e.g. ‘after all I said last time’, ‘I mean’, ‘and then where will she be’)
Swearwords (e.g. ‘it’s bloody awful’)
Tone of voice , such as extra loudness or long pauses followed by a strongly expressed phrase (Healy & Mulholland, 2007)
The guiding principle for deciding what information should be included in a case note is whether it is relevant to the service or support being provided. The type of information that is considered relevant may include:
a range of biopsychosocial, environmental and systemic factors impacting on the client; this includes consideration of an individual's culture, religion and spirituality
risk and resilience factors
facts, theory or research underpinning an assessment
a record of all discussions and interactions with the client and persons/services involved in the provision of support including referral information, telephone and email correspondence
a record of non-attendance, either by the Social Worker or client, at scheduled and agreed meetings or activities
evidence that the Social Worker and client have discussed their respective legal and ethical responsibilities. This may include:
client rights, responsibilities and complaints processes
the parameters of the service and support being offered and agreed to
issues relating to informed consent, information sharing, confidentiality and privacy
efforts to promote and support client self-determination and autonomy
specific responsibilities to clients in particular settings such as private practice or rural settings as per the relevant Association’s Code of Ethics document
professional boundaries and how dual relationships may be managed
record keeping and freedom of information
discharge planning
relevant legislative requirements and their possible implications for practice
details of reasons and any related actions or outcomes leading up to or following the termination or interruption of a service or support (AASW, 2016). Professional views may often be missing in case notes because social workers position their own subjectivity as irrelevant, or as threatening the achievement of accuracy and comprehensiveness. However, at times it is important to express it, e.g. where it is needed to justify an action (Lillis, 2017).
Other writers provide their own details of what should be included in case notes. In particular Oranga Tamariki (2022a) (the New Zealand Ministry for Children) provides general points when writing case notes. TheraNest (2020) draws together three sources to present a detailed list. This information is included under each of the references in the Supporting Material/References section that concludes this topic.
How should information be presented?
There are a number of case-writing models available to social workers. Some of them provide general guidance for writing case notes while others are specific to a service type or context. In addition, many organisations have policies and procedures around case recording (AASW, 2016). Case note templates are discussed further in the Practice Approach section that follows.
Sommers-Flanagan (2009) suggests the following should be used to structure case notes:
Most reports begin with identifying the reason for referral.
They then examine specific behavioural observations made by the interviewer.
The client’s specific problem is stated in some detail, along with its unique evolution. The history and description of several problems may be included.
For some clients past treatments or history of counselling can be listed.
Relevant medical history should be included, e.g. general health, recent illnesses, chronic physical illnesses or hospitalizations, prescription medications.
Include a social and family history where relevant.
Current ability to manage activities around daily living (ADLs) should be mentioned where relevant. This section can be expanded to include a description of the client’s psychological functioning, cognitive functioning, emotional functioning, or personality functioning.
Include some discussion of diagnostic issues, even if they are broad (e.g. depression, anxiety, substance use, eating disorder). For some clients, more detail may be appropriate.
Include a paragraph around case formulation and treatment plan: how the worker views the case and how the worker is likely to proceed in working with the client.
Can case notes be amended or changed at a later date?
If a change must be made to correct an error or omission, the change can be recorded as a new and separate case note. It is advisable to provide an explanation for its earlier absence or inaccuracy. Add, if possible, a note in the margin of the original case note referring the reader to the additional or amended detail (AASW, 2016).
What are the legislative responsibilities with regard to case notes?
Case notes may be subject to, and can be subpoenaed, for a range of legislative processes and requirements. The nature of these requirements may differ between organisations, districts, States and countries. Therefore it is important for Social Workers to:
be familiar with the specific legal requirements and processes impacting on practice
consider the implications of Federal and State legislation to the recording of case notes
understand how these requirements are implemented within their organisation (where relevant)
understand what policies and procedures may need to be implemented when working in private practice (AASW, 2016).
What should happen with case notes on termination of a service or support?
Termination or interruption of services should be included in case notes. Given termination may be unanticipated (e.g. departure of a social worker), it is particularly important to ensure that case notes are maintained and updated as soon after an interaction or event as practicable (AASW, 2016).
Sharing case notes with the client
It is important that clients can view reports, but they may also misinterpret information in a report unless offered guidance. The following guidelines are suggested:
Inform clients at the outset that records will be kept, and clients can have access to them.
Inform clients that some portions of the records are written in language designed to communicate with other professionals; consequently, the records may not be especially easy to read or understand.
If clients request their records, tell them you would like to review the records with them before releasing them, so as to minimize the possibility that the records are misinterpreted.
When clients request records, schedule an appointment (free of charge) with them to review the records together.
If clients are no longer seeing you, are angry with you, or refuse to meet with you, you can (a) release the records to them without a meeting (and hope the records are not misinterpreted), or (b) agree to release the records only to another licensed professional (who will review them with the client).
Whatever the situation, always discuss the issue of releasing records with your supervisor, rather than acting impulsively on your client's request (Sommers-Flanagan, 2009).
- Practice Approach
One of the themes to emerge from the literature around case notes is how they are “setting dependent” (AASW, 2016); Maple, 2012; TheraNest, 2020). Prescribed rules for what is included or excluded varies from agency to agency. However a number of key points from the Background Material section above. They include the following:
Each page should have the client's name, client's date of birth, social worker’s name and date of the interaction.
Case notes should be written as soon as possible after the interaction.
Consider who is going to read notes and how this should impact on writing style.
Information about a client should be impartial, accurate, complete, and free from emotive language.
Subjective opinions should be qualified with relevant background information, theory or research.
Be clear and consistent – don’t include extra details that are not to the point.
Sign and date the case notes when completed
Relevant information recorded in case notes may include:
The reason for the referral; the client’s specific problems
Evidence that legal and ethical responsibilities of both worker and client have been discussed
Relevant behavioural observations
A range of biopsychosocial, environmental and systemic factors impacting on the client. When relevant:
medical history
social and family history
ability to manage activities of daily living
culture, religion and spirituality
Risk and resilience factors
An assessment supported by facts, theory and/or research
A plan of action based on this assessment
A Selection of Formats for Writing Case Notes
Several different formats exist for writing case notes. TheraNest (2020) highlights three:
S.O.A.P. (Subjective, Objective, Assessment, Plan
D.A.P. (Data, Assessment, Plan)
B.I.R.P. (Behavior, Interventions, Response, Plan)
SOAP (Subjective, Objective, Assessment, Plan)
These four sections try to ensure case notes are complete, yet concise.
Subjective: What the client says about the problem; opinion-based information from the client including their goals, concerns, feelings, perceptions of their own problems. Also include relevant information from other family members or close friends.
Objective: Information that is fact-based, verifiable and quantifiable. This can be direct observations of the client. This might include things like the client’s appearance, body language and other obvious behaviour.
Assessment: Using subjective and objective information to assess the situation; a conclusion or recommendation could be included, with evidence as to why conclusions have been drawn.
Plan: The plan of action, e.g. referrals to other agencies, goals, timeline targets, i.e. the steps to take to assist the client meet their needs (AGS, 2019; Government of Northwest Territories Canada, n.d.; Moore, 2022a).
AGS (2019) provides two examples of case notes to illustrate the above. The AGS website also provides a template social workers can use to record case notes.
Examples of SOAP case notes
| what the client says | ||
| facts and observations | ||
| assess the situation + conclusion | ||
| steps to take; referrals | ||

DAP (Data, Assessment, Plan)
The Data heading covers everything that occurred during a counselling session, including but not limited to a client’s observable responses, affect, traits, and behavior. This section includes specific, objective information about the session’s focus, what was said, and more, in order to answer the question: “What did I observe?”
Under Assessment, social workers interpret and analyze the data in the previous session. This involves applying some professional subjectivity and may result in clinical hypotheses or findings. Here, social workers might record things like how a session related to a client’s overall treatment goals, a working hypothesis, and/or a probable diagnosis of a client’s condition.
The Plan section is used for making decisions and recommending a plan of treatment for the client. Here, the objective and subjective data from the previous two sections are used to inform a social worker’s strategy or next actions – often between the current session and the next. This could include recommendations for therapy or lifestyle changes, among other short- and long-term treatments (Moore, 2022b).
The key difference between SOAP and DAP formats is that the former breaks down the information about a session into two discrete sections, which can be highly useful in healthcare contexts where medications, blood results, and other clinical data can inform a patient’s treatment (Moore, 2022b).
BIRP (Behaviour, Interventions, Response, Plan)
Behavior (Presenting the Problem) This section records the subjective and objective details that were observed (CF SOAP outline above). This section can also contain details about the session itself, such as where it took place.
Example: Met with client X in the office. The most recent assessment shows they are presenting symptoms of anxiety. Today they showed signs of exhaustion, lack of focus, and looked tired. They reported not being able to sleep in the past week and feeling overwhelmed by work.
Interventions This section outlines the methods used to reach the goals and objectives of the therapy. It’s a concise summary of the conversation, focusing strongly on the therapist’s actions and the patient’s reactions.
Example: Through client-centered techniques, this writer encouraged the patient to expand their thoughts about their work. Negative thoughts were identified and challenged. The patient was asked to see if there is a link between their insomnia and the stressful period at work. The connection was successfully made and normalized through discussion. The conversation then focused on the specific work-related triggers that may have led to insomnia. A mild sleep aid was prescribed.
Response In this section, the therapist should record the client’s response to the intervention, including what the client said and how they reacted.
Example: The patient initially rejected the link between their insomnia and stress at work. When asked how work made them feel, the patient became silent, reduced eye contact, and disengaged from the conversation with the writer. After a few moments of thinking, the patient was able to describe their own feelings in relation to their work.
Plan The plan outlines when the next session will take place, and its focus.
Example: The next appointment scheduled for September 16, will assess the client’s response to the sleep aid and reassess their feelings about work.
https://quenza.com/blog/girp-notes/
The GIRP framework offers a powerful communication tool by delivering a streamlined, concise, and organized account of a patient or client’s journey. GIRP notes highlight key developments and treatment plans , becoming an invaluable asset for all stakeholders.
What is a GIRP note?
The acronym GIRP stands for: G oal, I ntervention, R esponse, and P lan.
Goal GIRP notes always start with a goal. The goal describes what the patient wants to get out of therapy or coaching. You might include both short and long-term goals in this first section. For example: Janine has been attending fortnightly psychotherapy sessions to get better control of her social anxiety and agoraphobia. Long-term, she would like to have a more active social life. However, at present, her main goal is to start doing her grocery shopping in person again. Janine feels this is a safe and achievable goal for her to build some positive momentum.
Intervention The intervention simply describes the techniques, methods, or strategies the practitioner and client are using to work toward the desired change.
So, in Janine’s case, the intervention section might read: Therapist and client discussed gradual exposure techniques to start working up to completing a full in-person grocery shop. Or, for another person: Discussed client’s limiting beliefs around her capacity to successfully launch an online business. Introduced the concept of focusing on strengths rather than weaknesses. Then, prompted the client to come up with some empowering affirmations she can use when self-doubt is becoming an issue.
Response The response section provides an objective account of the individual’s reaction or progress in response to the intervention. This forces the practitioner to hone in on whether what they are doing in session is working and adjust course if necessary. In coaching, an example would be: Client struggled immensely with identifying strengths. By the end of the session we identified 3: creativity, persistence, and ability to learn new things. Did not get to move onto affirmations before the end of the session.
Plan The plan sets out the forthcoming steps, giving a clear roadmap for future treatment, services, and/or client tasks, based on insights gained from the individual’s response to past interventions.
For example: Janine to undertake 2 more trips for grocery shopping before next session. If successful, therapist and patient to decide on a new goal. May be suitable to include more social interaction, in line with long-term goal of having an active social life.
Benefits of GIRP Notes
The two most significant benefits of GIRP notes are that they:
1. Enhance communication between the client and professionals involved in a case resulting in a collaborative approach to care and a strong therapeutic relationship.
2. Maintain a focus on the individual’s goals.
Biopsychosocial-Spiritual Approach (BPSS)
The BPSS is used quite frequently by social workers, especially in their initial dealings with clients. The following is a template that could be adapted as necessary for different clients. Other templates for the BPSS can be found in a separate topic on this website at https://www.thesocialworkgraduate.com/post/bio-psychosocial-spiritual-assessment
_________________________________________________________________________________
Client Name:
Client D.O.B:
Client address:
Client contact details:
Referred by:
Presenting problem:
Family Structure/genogram:
Medical / psychological history:
Current medications:
Employment / education:
Other issues: Should check areas in BPSS to see if any other topics should be included
Planned intervention and referrals:
_____________________________________________________________________________

Pacheco (2014) suggests social workers can develop a template that can be written over when taking notes.The template can contain prompts to ensure the social worker does not forget to touch on certain areas. An example using the BPSS approach is shown on the right.
This is quite simple to make: type up your page with the prompts, highlight the prompts, and choose a light colour from the available font colours, e.g.tan background 2.
Pacheco’s approach could be used with other approaches too, such as SOAP, DAP and BIRP.
A number of other writers suggest case notes templates, and these have been included under their reference in the following Supporting Material / References section.
Healy and Mulholland (2007) suggest three approaches: topic sentences, problems to be solved, and expressing client concerns.
Oranga Tamariki (2022b) provide an example of a good and poor case note
Social Work Haven (2021) has developed a case notes cheat sheet
Sommers-Flanagan (2009) provide a detailed intake report template.
Supporting Material/References
AASW: Australian Association of Social Workers. (2016). Case notes . Retrieved from https://www.aasw.asn.au/document/item/2356
AGS: Airiodion Global Services. (2019). A simple (but detailed) guide on different types & stages of social work processes . Retrieved frpm https://www.airiodion.com/social-work-process/
Healy, K., & Mulholland, J. (2007). Writing Case Records. In K Healy & J Mulholland (Eds.), Writing Skills for Social Workers (pp. 68-86) . Sage Publications.
Three Methods for Writing Case Notes
Topic sentences—provide the gist but leave out the detail
Problems to be solved
Expressing client concerns—state the client’s concerns as well as the social worker’s professional judgement
An example of each of the above follows based on this situation: The grandmother said: It was last Friday she came round, late as usual, and she hadn’t brought me any money to buy food for the kid after all I said last time it happened - no money and no food either - I mean I don’t mind looking after the kid - it’s bloody awful the way she treats that child - but on my pension I can’t pay for its food and that - I mean if she doesn’t give me some money soon I will have to stop caring for the kid and then where will she be?’
Topic sentences :
This case is about childcare by grandmother. Grandmother is client. The mother is in paid employment; she finds it difficult to supply money to the carer, and to pick up the child on time. The carer is unhappy about the money situation, and to lesser degree the time problem, and threatens to stop the caring.
Problems to be solved :
This case is about childcare by grandmother. Problem 1 - money, since mother is erratic about providing it.
Problem 2 - time of child collection, since mother is often late.
Problem 3 - carer is unhappy about the money situation, and to a lesser degree the time problem, and threatens to stop the caring.
[You may wish to go one step further and alert the attention of a specific team member by writing Problem 3 as : Problem 3 - ’In my view, the carer may need counselling’ , or ’Carer and mother may need mediation’.]
Expressing client concerns :
Client, grandmother as carer, complained about child’s mother supplying no money and being late. She warned that she could not continue with the childcare unless she was paid.
Lillis, T. (2017). Imagined, prescribed and actual text trajectories: The ‘problem’ with case notes in contemporary social work. Text and Talk, 37 (4), 485–508. http://dx.doi.org/doi:10.1515/text-2017-0013
Government of Northwest Territories Canada. (n.d.). SOAP case notes guide . Retrieved from https://www.hss.gov.nt.ca/professionals/sites/professionals/files/resources/soap-case-notes-guide.pdf
GoodTherapy. (2020). For social workers: Tips for writing case notes . Retrieved from https://www.goodtherapy.org/for-professionals/business-management/private-practices/article/for-social-workers-tips-for-writing-case-notes
Maple, M. (2012). Case notes . Lecture notes, HSSW 100, University of New England, Australia.
Miller, K. (2022). BIRP notes: A complete guide on the BIRP note-taking forma t. Retrieved from https://quenza.com/blog/birp-notes/
Moore, C. (2022a). Writing SOAP notes, step-by-step: Examples + templates . Retrieved from https://quenza.com/blog/soap-note/
Moore, C. (2022b). How to write DAP notes: 5 best templates and examples . Retrieved from https://quenza.com/blog/dap-notes/
Oranga Tamariki (New Zealand Ministry for Children). (2022a). Keeping accurate records – guidance . Retrieved from https://practice.orangatamariki.govt.nz/practice-approach/practice-standards/keep-accurate-records/keep-accurate-records-guidance/
Oranga Tamariki - New Zealand Ministry for Children (2022a) suggests the following general points in providing guidance for social workers when writing case records. Each point below is expanded in the actual document.
Implement the practice standards for each tamaiti (child) in case notes, assessments, plans and reports
Record the process of engaging with, assessing, making decisions and reasons for decisions
Ensure what is recorded is easily understood
Provide adequate support if tamariki (children) want access to records
Keep personal information safe and secure
Document any key decisions made, or actions taken, the rationale for decisions or actions and the next steps.
Records identify the key people with whom engagement has occurred
Document views on relevant people involved in the case and how this has informed decision-making
Develop a chronology of critical key events and changes for te tamaiti (the child) and whanau (family) across their lifespan
Document how tamaiti (child), their whanau (extended family), caregivers or others working with the have responded to social worker decisions
Choose an appropriate communicate approach when communicating with clients
Include in notes how the family responds to decisions made
Document any oversight/approval obtained for key decisions that require it
Record discussions, key points and decisions made during supervision or case consults, including next steps
Review records often to keep the current and accurate
Oranga Tamariki (New Zealand Ministry for Children). (2022b). Case note examples . Retrieved from https://practice.orangatamariki.govt.nz/previous-practice-centre/policy/recording/key-information/case note-examples/
| Date: d/m/y Venue: home address John Last-name (DOB d/m/y) Shirley Last-name (caregiver) Graeme Last-name (caregiver) – not home, at work. Name of social worker (Social Worker)
Ensuring John’s care placement is supported and meeting all his wellbeing needs.
John took me into his bedroom to show me all his toys and games. We played connect four and then cards. John talked about Jim (Paternal Grandfather) giving him the Sponge Bob cards for Christmas. John had good eye contact and was able to speak freely, chatting and answering questions. His hand eye coordination was great; John showed me how he could make a helicopter which then fired bullets. John talked about Fluffy (cat) and Peaches (dog). John showed me that Peaches will sit down on her blanket when John says “sit”. John talked about how much he loves rugby and can’t wait for the season to begin. John is hoping to have the same coach he had last year (called Wogs) because he really liked him. John said he likes playing touch at lunchtimes at school with his mates Daniel, Ethan, Dante, Jayden and Nikau. If there’s not a touch game on John usually plays basketball or tennis with his mates. John says he is happy seeing his mum. John didn’t expand on this topic.
Shirley had made afternoon tea; we sat at the dining room table together. John stayed in his room playing with his Lego. Shirley said she was “very happy” with how things were going and that John was a “good boy”.
John is playing cricket on Saturday mornings between 10am until 12pm. Graeme takes him to this and watches the games.
John is going well at school however his teacher is a bit concerned about his lack of concentration at times. The teacher said to Shirley that John daydreams a lot and when the teacher asks him what he is thinking about, he says rugby.
John still sees Tracey (mum) every Friday afternoon between 3.30 and 4.30pm at our office. Maggie (resource worker) picks John up from school and takes him to access, then drops him off at Shirley’s afterwards. Tom (Tracey’s partner) sometimes comes along to the visits with Tracey. No issues raised by Shirley.
Finances for John’s rugby subs and a pair of boots; Contact the school teacher to discuss John’s daydreaming, does this impact on his learning? Call Shirley/ Graham by (date), to organise the next home visit. Name Social Worker Office | Met with John and Shirley. John took me into his bedroom to show me all his toys and games. We sat on the floor and played Connect Four and then had a game of snap with some Sponge Bob cards John had got for Christmas from Jim. John then showed me a lego set he had where you can make trucks, cars, motorbikes and even a helicopter. John showed me how he could make the helicopter which then fired bullets. John also showed me Shirley’s cat, Fluffy and Dog, Peaches that he likes. John showed me that Peaches will sit down on her blanket when John says “sit”. Shirley had made afternoon tea, so we then sat at the huge dining room table and had scones with jam and cream and a cup of tea. Shirley said she was very happy with how things were going, and that John was a good boy. He is playing cricket on Saturday mornings at 10am and this goes until 12pm. Graeme takes him to this and watches the games. Shirley wanted to know if we could pay for John’s upcoming rugby subs and a pair of boots. Shirley wants to get John a good pair of Nike boots from Rebel Sport that will last the distance rather than cheap ones from the Warehouse that will fall apart halfway through the season. Shirley also said that John is going well at school however his teacher is a bit concerned about his lack of concentration at times. The teacher at KVPS has said that John daydreams a lot and when the teacher asks him what he is thinking about, he says rugby. John really loves rugby and can’t wait for the season to begin. John wants to have the same coach he had last year; a guy called Wogs who John really liked. John said he likes playing touch at lunchtimes at school with his mates Daniel, Ethan, Dante, Jayden and Nikau. If there’s not a touch game on John usually plays basketball or tennis with his mates. John still sees Tracey every Friday afternoon between 3.30 and 4.30pm at our office. Maggie picks John up from school and takes him to access, then drops him off at Shirley’s afterwards. Tom sometimes comes along to the visits with Tracey. I thanked Shirley for the afternoon tea and told her I’d be back in a couple of months. |
Pacheco, I. (2014). Note taking templates for clinical social work . Retrieved from http://socialworktech.com/2014/06/23/note-taking-templates-for-clinical-social-work/
Social Work Haven. (2021). Sample case notes from social work you can learn from . Retrieved from https://socialworkhaven.com/sample-case-notes-for-social-work/
Case notes cheat sheet
Date and time
Reason for contact or conversation
Capacity to make decisions around subject being discussed if applicable
Views of the person
Views of others
What did you see?
What did you do?
Any risks identified
Did you consult or share information with anyone? If so, why?
Your professional opinion and analysis
Action plan
Somers-Flanagan, J., & Sommers-Flanagan, R. (2009). Intake interviewing and report writing. In J. Sommers-Flanagan & R. Sommers-Flanagan (Eds.). Clinical interviewing (4th ed., 175-212). John Wiley & Sons.
Sample Intake Report Outline
Use the following intake report outline as a guide for writing a thorough intake report. Keep in mind that this outline is lengthy and therefore, in practical clinical situations, you will need to select what to include and what to omit in your client reports.
--------------------------------------------------------------
NAME: DATE OF BIRTH: AGE: DATE OF INTAKE: INTAKE INTERVIEWER: DATE OF REPORT:
I. Identifying Information and Reason for Referral
A. Client name
D. Racial/Ethnic information
E. Marital status
F. Referral source (and telephone number, when possible)
G. Reason for referral '(why has the client been sent to you for a consultation/intake session?)
H. Presenting complaint (use a quote from me client to describe the complaint)
II. Behavioral Observations (and Mental Status Examination)
A. Appearance upon presentation (including comments about contact, body posture, and facial expression)
B. Quality and quantity of speech and responsivity to questioning
C. Client description of mood (use a quote in the report when appropriate)
D. Primary thought content (including presence or absence of suicidal ideation)
E. Level of cooperation with the interview
F. Estimate of adequacy of the data obtained
III. History of the Present Problem (or iIlness)
A. Include one paragraph describing the client's presenting problems and associated current stressors
B. Include one or two paragraphs outlining when the problem initially began and the course or development of symptoms
C. Repeat, as needed, paragraph-long descriptions of additional current problems identified during the intake interview (client problems are usually organized using diagnostic-DSM-groupings, however, suicide ideation, homicide ideation, relationship problems, etc., may be listed)
D. Follow, as appropriate, with relevant negative or rule-out statements (e.g., with a clinically depressed client, it is important to rule out mania: "The client denied any history ofmanic episodes.")
IV. Past Treatment (Psychiatric) History and Family Treatment (Psychiatric) History
A. Include a description of previous clinical problems or episodes not included in the previous section (e.g., if the client is presenting with a problem of clinical anxiety, but also has a history of treatment for an eating disorder, the eating disorder should be noted here)
B. Description of previous treatment received, including hospitalization, medications, psychotherapy or counselling, case management, and so on.
C. Include a description of all psychiatric and substance abuse disorders found in all blood relatives (i.e., at least parents, siblings, grandparents, and children, but also possibly aunts, uncles, and cousins)
D. Also include a list of any significant major medical disorders in blood relatives (e.g., cancer, diabetes, seizure disorders, thyroid disease)
V. Relevant Medical History
A. List and briefly describe past hospitalizations and major medical illnesses (e.g., asthma, mv positive, hypertension)
B. Include a description of the client's current health status (it's good to use a client quote or physician quote here)
C. Current medications and dosages
D. Primary care physician (and/or specialty physician) and telephone numbers
VI. Developmental History (This section is optional and is most appropriate for inclusion in child/adolescent cases.)
VII. Social and Family History
A. Early memories/experiences (including, when appropriate, descriptions of parents and possible abuse or childhood trauma)
B. Educational history
C. Employment history
D. Military history
E. Romantic relationship history
F. Sexual history
G. Aggression/Violence history
H. Alcohol/Drug history (if not previously covered as a primary problem area)
I. Legal history
J. Recreational history
K. Spiritual/Religious history
VIII. Current situation and Functioning
A. A description of typical daily activities
B. Self-perceived strengths and weaknesses
C. Ability to complete normal activities of daily living
IX. Diagnostic Impressions (This section should include a discussion of diagnostic issues or a listing of assigned diagnoses.)
A. Brief discussion of diagnostic issues
B. Multiaxial diagnosis from DSM
X. Case Formulation and Treatment Plan
A. Include a paragraph description of how you conceptualize the case. This description will provide a foundation for how you will work with this per- son. For example, a behaviorist will emphasize reinforcement contingencies that have influenced the client's development of symptoms and that will likely aid in alleviation of client symptoms. Alternatively, a psycho- analytically oriented interviewer will emphasize personality dynamics and historically significant and repeating relationship conflicts.
B. Include a paragraph description (or list) of recommended treatment approaches.
TheraNest. (2020). Elements of effective case notes for social wor k. Retrieved from https://theranest.com/blog/elements-of-effective-case-notes-for-social-work/
The guiding principle for writing effective case notes is to include content relevant to the service(s) or support provided. The specific content will vary based on your specific situation, but AASW broadly recommends the following:
The biopsychosocial, environmental and systemic factors impacting the client, including the client’s culture, religion/spirituality
Facts, theory or research underpinning an assessment
A record of all discussions and interactions with the client and persons/services involved in the provision of support including referral information, telephone and email correspondence
A record of non-attendance (by either you or your client) at scheduled and agreed meetings or activities
Evidence that you and your client have discussed your respective legal and ethical responsibilities — such as client rights and responsibilities, informed consent, confidentiality and privacy, professional boundaries, freedom of information, etc.
In addition to these broad guidelines, experts also recommend including the following specific pieces of information in each case note:
Topics discussed during the session
How the session related to the treatment plan
How the treatment plan goals and objectives are being met
Interventions and techniques used during the session and their effectiveness
Clinical observations
Progress or setbacks
Signs, symptoms and any increase or decrease in the severity of behaviors as they relate to any diagnosis used
Homework assigned, results and compliance
The client’s current strengths and challenges
Additionally, the following have to be included in case notes:
Demographic information
Prognosis and treatment plan
Progress to date
Dates of service
Who attended the sessions
Financial issues (billing, costs, payments, etc.)
This may seem like a lot of information to present, but case notes with this data will help document not only what took place in the session, but also your decision-making process and how you implemented treatment and intervention
Recent Posts
An Everyday Social Work Approach
Bio-Psychosocial-Spiritual Assessment
A sample case study: Mrs Brown
On this page, social work report, social work report: background, social work report: social history, social work report: current function, social work report: the current risks, social work report: attempts to trial least restrictive options, social work report: recommendation, medical report, medical report: background information, medical report: financial and legal affairs, medical report: general living circumstances.
This is a fictitious case that has been designed for educative purposes.
Mrs Beryl Brown URN102030 20 Hume Road, Melbourne, 3000 DOB: 01/11/33
Date of application: 20 August 2019
Mrs Beryl Brown (01/11/33) is an 85 year old woman who was admitted to the Hume Hospital by ambulance after being found by her youngest daughter lying in front of her toilet. Her daughter estimates that she may have been on the ground overnight. On admission, Mrs Brown was diagnosed with a right sided stroke, which has left her with moderate weakness in her left arm and leg. A diagnosis of vascular dementia was also made, which is overlaid on a pre-existing diagnosis of Alzheimer’s disease (2016). Please refer to the attached medical report for further details.
I understand that Mrs Brown has been residing in her own home, a two-story terrace house in Melbourne, for almost 60 years. She has lived alone since her husband died two years ago following a cardiac arrest. She has two daughters. The youngest daughter Jean has lived with her for the past year, after she lost her job. The eldest daughter Catherine lives on the Gold Coast with her family. Mrs Brown is a retired school teacher and she and both daughters describe her as a very private woman who has never enjoyed having visitors in her home. Mrs Brown took much encouragement to accept cleaning and shopping assistance once a week after her most recent admission; however, she does not agree to increase service provision. Jean has Enduring Power of Attorney (EPOA) paperwork that indicates that Mrs Brown appointed her under an EPOA two years ago. She does not appear to have appointed a medical treatment decision maker or any other decision-supporter.
I also understand from conversations with her daughters that Jean and Mrs Brown have always been very close and that there is a history of long-standing conflict between Catherine and Jean. This was exacerbated by the death of their father. Both daughters state they understand the impact of the stroke on their mother’s physical and cognitive functioning, but they do not agree on a discharge destination. Mrs Brown lacks insight into her care needs and says she will be fine once she gets back into her own home. Repeated attempts to discuss options with all parties in the same room have not resulted in a decision that is agreeable to all parties.
Mrs Brown has a history of Alzheimer’s disease; type II diabetes – insulin dependent; hypertension; high cholesterol and osteoarthritis. She has had two recent admissions to hospital for a urinary tract infection and a fall in the context of low blood sugars. She is currently requiring one to two people to assist her into and out of bed and one person with managing tasks associated with post-toilet hygiene. She can walk slowly for short distances with a four-wheel frame with one person to supervise. She benefits from prompting to use her frame; she needs someone to cut her food and to set her up to eat and drink regularly and to manage her medication routine. She requires one person to assist her to manage her insulin twice daily.
The team believe that Mrs Brown’s capacity for functional improvement has plateaued in the last ten days. They recommend that it is in her best interests to be discharged to a residential care setting due to her need for one to two people to provide assistance with the core tasks associated with daily living. Mrs Brown is adamant that she wants to return home to live with Jean who she states can look after her. Jean, who has a history of chronic back pain, has required several admissions to hospital over the past five years, and states she wants to be able to care for her mother at home. Jean states she is reluctant to agree to extra services as her mother would not want this. Her sister Catherine is concerned that Jean has not been coping and states that given this is the third admission to hospital in a period of few months, believes it is now time for her mother to enter residential care. Catherine states that she is very opposed to her mother being discharged home.
Mrs Brown is at high risk of experiencing falls. She has reduced awareness of the left side of her body and her ability to plan and process information has been affected by her stroke. She is now requiring one to two people to assist with all her tasks of daily living and she lacks insight into these deficits. Mrs Brown is also at risk of further significant functional decline which may exacerbate Jean’s back pain. Jean has stated she is very worried about where she will live if her mother is to enter residential care.
We have convened two family meetings with Mrs Brown, both her daughters and several members of the multi-disciplinary team. The outcome of the first meeting saw all parties agree for the ward to provide personalised carer training to Jean with the aim of trialling a discharge home. During this training Jean reported significant pain when transferring her mother from the bed and stated she would prefer to leave her mother in bed until she was well enough to get out with less support.
The team provided education to both Jean and Catherine about the progressive impact of their mother’s multiple conditions on her functioning. The occupational therapist completed a home visit and recommended that the downstairs shower be modified so that a commode can be placed in it safely and the existing dining room be converted into a bedroom for Mrs Brown. Mrs Brown stated she would not pay for these modifications and Jean stated she did not wish to go against her mother’s wishes. The team encouraged Mrs Brown to consider developing a back-up plan and explore residential care options close to her home so that Jean could visit often if the discharge home failed. Mrs Brown and Jean refused to consent to proceed with an Aged Care Assessment that would enable Catherine to waitlist her mother’s name at suitable aged care facilities. We proceeded with organising a trial overnight visit. Unfortunately, this visit was not successful as Jean and Catherine, who remained in Melbourne to provide assistance, found it very difficult to provide care without the use of an accessible bathroom. Mrs Brown remains adamant that she will remain at home. The team is continuing to work with the family to maximise Mrs Brown’s independence, but they believe that it is unlikely this will improve. I have spent time with Jean to explore her adjustment to the situation, and provided her with information on community support services and residential care services. I have provided her with information on the Transition Care Program which can assist families to work through all the logistics. I have provided her with more information on where she could access further counselling to explore her concerns. I have sought advice on the process and legislative requirements from the Office of the Public Advocate’s Advice Service. I discussed this process with the treating team and we decided that it was time to lodge an application for guardianship to VCAT.
The treating team believe they have exhausted all least restrictive alternatives and that a guardianship order is required to make a decision on Mrs Brown’s discharge destination and access to services. The team recommend that the Public Advocate be appointed as Mrs Brown’s guardian of last resort. We believe that this is the most suitable arrangement as her daughters are not in agreement about what is in their mother’s best interests. We also believe that there is a potential conflict of interest as Jean has expressed significant concern that her mother’s relocation to residential care will have an impact on her own living arrangements.
Mrs Brown’s medical history includes Alzheimer’s disease; type II diabetes; hypertension; high cholesterol and osteoarthritis. She was admitted to Hume Hospital on 3 March 2019 following a stroke that resulted in moderate left arm and leg weakness. This admission was the third hospital admission in the past year. Other admissions have been for a urinary tract infection, and a fall in the context hypoglycaemia (low blood sugars), both of which were complicated by episodes of delirium.
She was transferred to the subacute site under my care, a week post her admission, for slow-stream rehabilitation, cognitive assessment and discharge planning.
Mrs Brown was diagnosed with Alzheimer’s disease by Dr Joanne Winters, Geriatrician, in April 2016. At that time, Mrs Brown scored 21/30 on the Standardised Mini-Mental State Examination (SMMSE). During this admission, Mrs Brown scored 15/30. I have undertaken cognitive assessment and agree with the diagnosis; further cognitive decline has occurred in the context of the recent stroke. There are global cognitive deficits, but primarily affecting memory, attention and executive function (planning, problem solving, mental flexibility and abstract reasoning). The most recent CT-Brain scan shows generalised atrophy along with evidence of the new stroke affecting the right frontal lobe. My assessments suggest moderate to severe mixed Alzheimer’s and vascular dementia.
While able to recall some key aspects of her financial affairs, including the general monetary value of her pension and regular expenses, Mrs Brown was unable to account for recent expenditure (for repairs to her home) or provide an estimate of its value, and had difficulty describing her investments. In addition, I consider that she would be unable to make complex financial decisions due to her level of cognitive impairment. Accordingly, I am of the view that Mrs Brown now lacks capacity to make financial decisions.
Mrs Brown states that she previously made an Enduring Power of Attorney (EPOA) but could no longer recall aspects of the EPOA, such as when it would commence and the nature of the attorney’s powers. Moreover, she confused the EPOA with her will. Her understanding of these matters did not improve with education, and therefore I consider that she no longer has capacity to execute or revoke an EPOA.
Mrs Brown acknowledges that she needs some assistance but lacks insight into the type of assistance that she requires, apart from home help for cleaning and shopping. She does not appreciate her risk of falling. She is unable to get in and out of bed without at least one person assisting her. She frequently forgets to use her gait aid when mobilising and is not able to describe how she would seek help in the event of falling. She is not able to identify or describe how she would manage her blood sugar levels, and this has not improved with education. Accordingly, I consider that she lacks capacity to make decisions about accommodation arrangements and services.
Mrs Brown does not agree with the treating team’s recommendation to move into residential care and maintains her preference to return home. This is in spite of a failed overnight trial at home with both her daughters assisting her. Unfortunately, she was unable to get out of bed to get to the toilet and required two people to assist her to do so in the morning. In light of these matters, and in the context of family disagreement regarding the matter, the team recommends that the Office of the Public Advocate be appointed as a guardian of last resort.
Reviewed 22 July 2022
- Hospitals & health services
- Public hospitals in Victoria
- Patient care
- Ambulance and patient transport
- Non-emergency patient transport
- Non-emergency patient transport review
- NEPT legislation and clinical practice protocols
- Non-emergency patient transport licensing
- NEPT licensing fees
- NEPT services information and guidance
- First Aid Services
- First aid licences
- First aid services information and guidance
- First aid service fees
- Victorian State Trauma System
- Acute medicine
- Emergency care
- Surgical services
- Better at Home
- Critical care
- Hospital in the Home
- Virtual care (Telehealth)
- Perinatal and reproductive services
- Rehabilitation and complex care
- Renal health
- Renal services in Victoria
- Funding for renal services
- Different approaches to haemodialysis
- Specialist clinics
- Access to non-admitted services
- Minimum referral information
- Communication toolkit
- Integrated care
- HealthLinks: Chronic Care
- Community Health Integrated Program (CHIP) guidelines
- Service coordination in Victoria
- Victorian integrated care online resources
- Specialist clinics programs
- Specialist clinics reform
- Specialty diagnostics, therapeutics and programs
- Older people in hospital
- End of life and palliative care in Victoria
- Voluntary assisted dying
- Quality, safety and service improvement
- Planned surgery recovery and reform program
- Digital Health
- Roadmap and Maturity Model
- Standards and guidelines
- Policies and frameworks
- Health Information Sharing Legislation Reform
- My Health Record
- Public hospital accreditation in Victoria
- Credentialing for senior medical staff in Victoria
- Clinical risk management
- Preventing infections in health services
- Healthy choices
- Victorian Perinatal Data Collection
- Rural health
- Improving Access to Primary Care in Rural and Remote Areas Initiative
- Rural x-ray services
- Rural health regions and locations
- Rural and regional medical director role
- Victorian Patient Transport Assistance Scheme
- Rural and isolated practice registered nurses
- Urgent care in regional and rural Victoria
- Private health service establishments
- Private hospitals
- Day procedure centres
- Mobile health services
- Fees for private health service establishments in Victoria
- Design resources for private health service establishments
- Professional standards in private health service establishments
- Legislation updates for private health service establishments
- Complaints about private health service establishments
- Cosmetic procedures
- Guideline for providers of liposuction
- Private hospital funding agreement
- Boards and governance
- About health service boards in Victoria
- Information and education
- Education resources for boards
- Sector leadership
- Data, reporting and analytics
- Health data standards and systems
- Funding, performance and accountability
- Statements of Priorities
- Performance monitoring framework
- Integrity governance framework and assessment tool
- Pricing and funding framework
- Patient fees and charges
- Fees and charges for admitted patients
- Non-admitted patients - fees and charges
- Other services
- Planning and infrastructure
- Sustainability in Healthcare
- Medical equipment asset management framework
- Health system design, service and infrastructure planning
- Complementary service and locality planning
- Primary & community health
- Primary care
- Community pharmacist pilot
- EOI - Victorian Community Pharmacist Statewide Pilot
- Victorian Community Pharmacist Statewide Pilot – Resources for pharmacists
- Emergency Response Planning Tool
- Working with general practice
- Victorian Supercare Pharmacies
- NURSE-ON-CALL
- Priority Primary Care Centres
- Local Public Health Units
- Community health
- Community health services
- Community health pride
- Registration and governance of community health centres
- Community Health Directory
- Community Health Program in Victoria
- Community health population groups
- Dental health
- Access to public dental care services
- Victoria's public dental care fees
- Victoria's public dental care waiting list
- Dental health for SRS residents
- Dental health program reporting
- Smile Squad school dental program
- Maternal and Child Health Service
- Nursery Equipment Program
- Maternal and Child Health Service Framework
- Maternal and Child Health Service resources
- Child Development Information System
- Early parenting centres
- Maternal Child and Health Reporting, Funding and Data
- Baby bundle
- Sleep and settling
- Maternal and Child Health Workforce professional development
- Aboriginal Maternal and Child Health
- Public Dental and Community Health Program funding model review
- Public health
- Women's Health and Wellbeing Program
- Inquiry into Women's Pain
- Inquiry into Women's Pain submissions
- Support groups and programs
- About the program
- Victorian Women's Health Advisory Council
- Cemeteries and crematoria
- Medicines and Poisons Regulation
- Patient Schedule 8 treatment permits
- Schedule 8 MDMA and Schedule 8 psilocybine
- Schedule 9 permits for clinical trials
- Documents and forms to print or download
- Legislation and Approvals
- Frequently Asked Questions - Medicines and Poisons Regulation
- Health practitioners
- Licences and permits to possess (& possibly supply) scheduled substances
- Medicinal cannabis
- Pharmacotherapy (opioid replacement therapy)
- Recent updates
- Environmental health
- Improving childhood asthma management in Melbourne's inner west
- Climate and weather, and public health
- Environmental health in the community
- Environmental health in the home
- Environmental health professionals
- Face masks for environmental hazards
- Human health risk assessments
- Lead and human health
- Per- and poly-fluoroalkyl substances (PFAS)
- Pesticide use and pest control
- Food safety
- Information for community groups selling food to raise funds
- Food businesses
- Food safety information for consumers
- Food regulation in Victoria
- Food safety library
- Food allergens
- Introducing Standard 3.2.2A: Food safety management tools
- Immunisation
- Respiratory syncytial virus (RSV) immunisation
- Seasonal influenza vaccine
- Immunisation schedule and vaccine eligibility criteria
- Ordering vaccine
- Immunisers in Victoria
- Immunisation provider information
- Cold chain management
- Adverse events following immunisation reporting
- Vaccine error management
- Vaccination for infants and children
- Vaccination for adolescents
- Vaccination program for adults
- Vaccination for special-risk groups
- Immunisation resources order form
- Victorian coverage rates for Victoria
- Infectious diseases guidelines & advice
- Infection control guidelines
- Disease information and advice
- Advice to the cruise industry: reporting infections
- Notifiable infectious diseases, conditions and micro-organisms
- Notification procedures for infectious diseases
- Infectious diseases surveillance in Victoria
- Germicidal ultraviolet light
- Protecting patient privacy in Victoria
- Population health systems
- Evidence and evaluation
- Health promotion
- Health status of Victorians
- Municipal public health and wellbeing planning
- Population screening
- Cancer screening
- Conditions not screened
- Improving outcomes in under-screened groups
- Infant hearing screening
- Newborn bloodspot screening
- Prenatal screening
- Screening registers
- Preventive health
- Type 2 diabetes and cardiovascular disease prevention
- Eye health promotion
- Injury prevention
- Healthy eating
- Oral health promotion
- Physical activity
- Sexual health
- Sex worker health
- Decriminalisation of sex work
- Automatic mutual recognition
- Domestic smoke detectors
- Lasers, IPL and LED devices for cosmetic treatments and beauty therapy
- Victoria's regulatory framework for radiation
- Radiation newsletter
- Tobacco reforms
- Tobacco reform legislation and regulations
- E-cigarettes and vaping
- Quitting smoking and vaping
- Smoke-free and vape-free areas
- Building entrances
- Children's indoor play centres
- Public hospitals and health centres
- Children's recreational areas
- Playground equipment
- Skate parks
- Swimming pools
- Under-age sporting events
- Enclosed workplaces
- Government buildings
- Learning environments
- Outdoor dining
- Outdoor drinking areas
- Patrolled beaches
- Train platforms and bus and tram shelters
- Under-age music or dance events
- Tobacco and e-cigarette retailers
- Making a report or complaint
- Resources and factsheets
- Alternative water supplies
- Aquatic facilities
- Blue-green algae (cyanobacteria)
- Drinking water in Victoria
- Legionella risk management
- Private drinking water
- Recreational water use and possible health risks
- Water fluoridation
- Chief Health Officer
- About the Chief Health Officer
- Chief Health Officer publications
- Health alerts and advisories
- Mental health
- Mental Health and Wellbeing Act 2022
- Mental Health and Wellbeing Act 2022 Handbook
- Community information
- Mental Health and Wellbeing Act 2022 in your language
- About Victoria's mental health services
- Area-based services
- Statewide and specialist mental health services
- Mental Health Community Support Services
- Support and intervention services
- Language services - when to use them
- Access to mental health services across areas
- Transport for people in mental health services
- Practice and service quality
- Medical Treatment Planning and Decisions Act
- Service quality
- Specialist responses
- Mental health and wellbeing reform
- Reform activity updates
- Priority areas
- Latest news
- Working with consumers and carers
- Consumer and carer engagement
- Consumer and Carer Experience Surveys
- Family support and crisis plans
- Consumer and carer financial support
- Supporting children whose parents have a mental illness
- Supporting parents with a mental illness
- Prevention and promotion
- Early intervention in mental illness
- Mental health promotion in Victoria
- Suicide prevention in Victoria
- Priorities and transformation
- Supporting the social and emotional wellbeing of Aboriginal and Torres Strait Islander Victorians
- National mental health strategy
- Rights and advocacy
- Making a complaint about a mental health service
- Chief Psychiatrist
- About the Chief Psychiatrist
- Principles in the Mental Health and Wellbeing Act and the Chief Psychiatrist's guidelines
- Obligations under the Mental Health and Wellbeing Act 2022
- Reporting a failure to comply with the Mental Health and Wellbeing Act 2022
- Governance and committees
- Reporting obligations for clinical mental health and wellbeing services
- Mental health and wellbeing support
- Making a complaint and seeking advocacy
- Second psychiatric opinion and process of review by Chief Psychiatrist
- Office of the Chief Psychiatrist's reform activities and news
- Oversight of forensic mental health and wellbeing services
- Resources and reports
- Chief psychiatrist guidelines
- Chief Mental Health Nurse
- About Victoria's Chief Mental Health Nurse
- Best practice
- Reducing restrictive interventions
- Research and reporting
- Mental health performance reports
- Reporting requirements and business rules for clinical mental health services
- Alcohol & drugs
- Alcohol and other drug treatment services
- Overview of Victoria's alcohol and drug treatment system
- Pathways into alcohol and other drugs treatment
- Prevention and harm reduction
- Medically supervised injecting room
- Victoria's Take-Home Naloxone Program
- Community-based AOD treatment services in Victoria
- Residential treatment services
- Mildura statewide alcohol and drug residential treatment service
- Drug rehabilitation plan
- Hospital-based services
- Forensic services
- Pharmacotherapy treatment
- Services for Aboriginal people
- Services for young people
- Statewide and specialist services
- Compulsory treatment
- Family and peer support
- Public intoxication reform
- New public intoxication response services
- Policy, research and legislation
- Alcohol and drug research and data
- Legislation governing alcohol and other drug treatment
- Alcohol and other drug service standards and guidelines
- Alcohol and other drug client charter and resources
- Alcohol and other drug treatment principles
- Service quality and accreditation
- Alcohol and other drug program guidelines
- Maintenance pharmacotherapy
- Specialist Family Violence Advisor capacity building program in mental health and alcohol and other drug services - Victoria
- Alcohol and other drug workforce
- Learning and development
- Alcohol and other drug workforce Minimum Qualification Strategy
- Workforce data and planning
- Funding and reporting for alcohol and other drug services
- Funding of alcohol and other drugs services in Victoria
- Reporting requirements and business rules for alcohol and other drug services
- Drug alerts
- 25C-NBOMe and 4-FA sold as '2C-B'
- Novel stimulants sold as MDMA, cocaine or speed
- Protonitazene sold as ketamine
- High potency benzodiazepine tablets
- MDMA adulterated with PMMA
- 25B-NBOH sold as powdered 'LSD'
- Green 'UPS' pills containing N-ethylpentylone (no MDMA)
- N-ethylpentylone in cocaine
- Ageing & aged care
- Supporting independent living
- Low cost accommodation support programs
- Personal Alert Victoria
- Dementia services
- Victorian Aids and Equipment Program
- Residential aged care services
- Public sector residential aged care services
- Safety and quality in public sector residential aged care
- Physical and social environments
- Emergency preparedness in residential aged care services
- My Aged Care assessment services
- Home and Community Care Program for Younger People
- HACC data reporting
- HACC PYP fees policy and schedule of fees
- Wellbeing and participation
- Age-friendly Victoria
- Healthy ageing
- Seniors participation
- Dementia-friendly environments
- Designing for people with dementia
- Maintaining personal identity
- Personal enjoyment
- Interior design
- Dining areas, kitchens and eating
- Bedrooms and privacy
- Gardens and outdoor spaces
- Assistive technology
- Staff education and support
- Strategies, checklists and tools
- Our Strategic Plan 2023-27
- Our organisation
- Our secretary
- Leadership charter
- Our services
- Our vision and values
- Specialist offices
- Senior officers in health
- Human Research Ethics Committee (HREC)
- Gifts, benefits and hospitality policy
- Information Asset Register
- Health legislation
- Health legislation overview
- Health Complaints legislation
- Health Records Act
- Human Tissue Act 1982
- Public Health and Wellbeing Act 2008
- Voluntary Assisted Dying Act
- Victoria's pandemic management framework
- Independent Pandemic Management Advisory Committee
- Pandemic Order Register
- Our ministers
- Our role in emergencies
- State Health Emergency Response Arrangements
- Emergency type
- Department's responsibilities in emergencies
- Health services’ responsibilities in emergencies
- Aboriginal employment
- Current vacancies
- Employment programs for students and graduates
- Rise program
- Inclusion and diversity at the Department of Health
- Health workforce
- Working in health
- Information sharing and MARAM
- Child Safe Standards
- Regulatory functions
- Reviews of decisions
- Victorian Public Healthcare Awards
- Aboriginal healthcare workers
- Mental health workforce
- Lived and living experience workforces
- Engaging with lived and living experience workforces
- Our workforce, our future
- Nursing and midwifery
- Free nursing and midwifery study
- Additional funding for nursing and midwifery positions
- Becoming a nurse or midwife
- Undergraduate nursing and midwifery scholarships
- Undergraduate student employment programs
- Nursing and midwifery graduates
- Nursing and midwifery graduate sign-on bonus
- Working as a nurse or midwife
- Enrolled nurse to registered nurse transition scholarships
- Support for new nurse practitioners
- Postgraduate scholarships for nurses and midwives
- Nurse practitioners
- Returning to nursing or midwifery
- Refresher pathway for nurses and midwives
- Re-entry pathway scholarships for nurses and midwives
- Nursing and midwifery - legislation and regulation
- Nursing and midwifery program - health sector
- Allied health workforce
- Education and training
- Enterprise agreements
- Worker health and wellbeing
- Working with us
- Grants and programs
- Freedom of Information
- Part II - Information Statements
- Procurement policies
- Protective markings
- Health and medical research
- Sponsorship application information
- Publications
- Annual reports
- Fact sheets
- Strategies, plans and charters
- Policies, standards and guidelines
- Research and reports
- Forms and templates
- Communities
- Designing for Diversity
- Vulnerable children
- Vulnerable children - responsibilities of health professionals
- Identifying and responding to children at risk
- Pathway to good health for children in care
- Older people
- Aboriginal health
- Improving health for Victorians from culturally and linguistically diverse backgrounds
- Asylum seeker and refugee health in Victoria
- News and media hub
- Media releases
- Health alerts
- Feedback and complaints
- Make a payment
- Fees, charges and penalties subject to automatic indexation
- Our campaigns
Share this page
- Facebook , opens a new window
- X (formerly Twitter) , opens a new window
- LinkedIn , opens a new window
- Search Menu
Sign in through your institution
- Browse content in Arts and Humanities
- Browse content in Archaeology
- Anglo-Saxon and Medieval Archaeology
- Archaeological Methodology and Techniques
- Archaeology by Region
- Archaeology of Religion
- Archaeology of Trade and Exchange
- Biblical Archaeology
- Contemporary and Public Archaeology
- Environmental Archaeology
- Historical Archaeology
- History and Theory of Archaeology
- Industrial Archaeology
- Landscape Archaeology
- Mortuary Archaeology
- Prehistoric Archaeology
- Underwater Archaeology
- Urban Archaeology
- Zooarchaeology
- Browse content in Architecture
- Architectural Structure and Design
- History of Architecture
- Residential and Domestic Buildings
- Theory of Architecture
- Browse content in Art
- Art Subjects and Themes
- History of Art
- Industrial and Commercial Art
- Theory of Art
- Biographical Studies
- Byzantine Studies
- Browse content in Classical Studies
- Classical History
- Classical Philosophy
- Classical Mythology
- Classical Literature
- Classical Reception
- Classical Art and Architecture
- Classical Oratory and Rhetoric
- Greek and Roman Papyrology
- Greek and Roman Epigraphy
- Greek and Roman Law
- Greek and Roman Archaeology
- Late Antiquity
- Religion in the Ancient World
- Social History
- Digital Humanities
- Browse content in History
- Colonialism and Imperialism
- Diplomatic History
- Environmental History
- Genealogy, Heraldry, Names, and Honours
- Genocide and Ethnic Cleansing
- Historical Geography
- History by Period
- History of Emotions
- History of Agriculture
- History of Education
- History of Gender and Sexuality
- Industrial History
- Intellectual History
- International History
- Labour History
- Legal and Constitutional History
- Local and Family History
- Maritime History
- Military History
- National Liberation and Post-Colonialism
- Oral History
- Political History
- Public History
- Regional and National History
- Revolutions and Rebellions
- Slavery and Abolition of Slavery
- Social and Cultural History
- Theory, Methods, and Historiography
- Urban History
- World History
- Browse content in Language Teaching and Learning
- Language Learning (Specific Skills)
- Language Teaching Theory and Methods
- Browse content in Linguistics
- Applied Linguistics
- Cognitive Linguistics
- Computational Linguistics
- Forensic Linguistics
- Grammar, Syntax and Morphology
- Historical and Diachronic Linguistics
- History of English
- Language Evolution
- Language Reference
- Language Acquisition
- Language Variation
- Language Families
- Lexicography
- Linguistic Anthropology
- Linguistic Theories
- Linguistic Typology
- Phonetics and Phonology
- Psycholinguistics
- Sociolinguistics
- Translation and Interpretation
- Writing Systems
- Browse content in Literature
- Bibliography
- Children's Literature Studies
- Literary Studies (Romanticism)
- Literary Studies (American)
- Literary Studies (Asian)
- Literary Studies (European)
- Literary Studies (Eco-criticism)
- Literary Studies (Modernism)
- Literary Studies - World
- Literary Studies (1500 to 1800)
- Literary Studies (19th Century)
- Literary Studies (20th Century onwards)
- Literary Studies (African American Literature)
- Literary Studies (British and Irish)
- Literary Studies (Early and Medieval)
- Literary Studies (Fiction, Novelists, and Prose Writers)
- Literary Studies (Gender Studies)
- Literary Studies (Graphic Novels)
- Literary Studies (History of the Book)
- Literary Studies (Plays and Playwrights)
- Literary Studies (Poetry and Poets)
- Literary Studies (Postcolonial Literature)
- Literary Studies (Queer Studies)
- Literary Studies (Science Fiction)
- Literary Studies (Travel Literature)
- Literary Studies (War Literature)
- Literary Studies (Women's Writing)
- Literary Theory and Cultural Studies
- Mythology and Folklore
- Shakespeare Studies and Criticism
- Browse content in Media Studies
- Browse content in Music
- Applied Music
- Dance and Music
- Ethics in Music
- Ethnomusicology
- Gender and Sexuality in Music
- Medicine and Music
- Music Cultures
- Music and Media
- Music and Religion
- Music and Culture
- Music Education and Pedagogy
- Music Theory and Analysis
- Musical Scores, Lyrics, and Libretti
- Musical Structures, Styles, and Techniques
- Musicology and Music History
- Performance Practice and Studies
- Race and Ethnicity in Music
- Sound Studies
- Browse content in Performing Arts
- Browse content in Philosophy
- Aesthetics and Philosophy of Art
- Epistemology
- Feminist Philosophy
- History of Western Philosophy
- Metaphysics
- Moral Philosophy
- Non-Western Philosophy
- Philosophy of Language
- Philosophy of Mind
- Philosophy of Perception
- Philosophy of Science
- Philosophy of Action
- Philosophy of Law
- Philosophy of Religion
- Philosophy of Mathematics and Logic
- Practical Ethics
- Social and Political Philosophy
- Browse content in Religion
- Biblical Studies
- Christianity
- East Asian Religions
- History of Religion
- Judaism and Jewish Studies
- Qumran Studies
- Religion and Education
- Religion and Health
- Religion and Politics
- Religion and Science
- Religion and Law
- Religion and Art, Literature, and Music
- Religious Studies
- Browse content in Society and Culture
- Cookery, Food, and Drink
- Cultural Studies
- Customs and Traditions
- Ethical Issues and Debates
- Hobbies, Games, Arts and Crafts
- Natural world, Country Life, and Pets
- Popular Beliefs and Controversial Knowledge
- Sports and Outdoor Recreation
- Technology and Society
- Travel and Holiday
- Visual Culture
- Browse content in Law
- Arbitration
- Browse content in Company and Commercial Law
- Commercial Law
- Company Law
- Browse content in Comparative Law
- Systems of Law
- Competition Law
- Browse content in Constitutional and Administrative Law
- Government Powers
- Judicial Review
- Local Government Law
- Military and Defence Law
- Parliamentary and Legislative Practice
- Construction Law
- Contract Law
- Browse content in Criminal Law
- Criminal Procedure
- Criminal Evidence Law
- Sentencing and Punishment
- Employment and Labour Law
- Environment and Energy Law
- Browse content in Financial Law
- Banking Law
- Insolvency Law
- History of Law
- Human Rights and Immigration
- Intellectual Property Law
- Browse content in International Law
- Private International Law and Conflict of Laws
- Public International Law
- IT and Communications Law
- Jurisprudence and Philosophy of Law
- Law and Politics
- Law and Society
- Browse content in Legal System and Practice
- Courts and Procedure
- Legal Skills and Practice
- Primary Sources of Law
- Regulation of Legal Profession
- Medical and Healthcare Law
- Browse content in Policing
- Criminal Investigation and Detection
- Police and Security Services
- Police Procedure and Law
- Police Regional Planning
- Browse content in Property Law
- Personal Property Law
- Study and Revision
- Terrorism and National Security Law
- Browse content in Trusts Law
- Wills and Probate or Succession
- Browse content in Medicine and Health
- Browse content in Allied Health Professions
- Arts Therapies
- Clinical Science
- Dietetics and Nutrition
- Occupational Therapy
- Operating Department Practice
- Physiotherapy
- Radiography
- Speech and Language Therapy
- Browse content in Anaesthetics
- General Anaesthesia
- Neuroanaesthesia
- Clinical Neuroscience
- Browse content in Clinical Medicine
- Acute Medicine
- Cardiovascular Medicine
- Clinical Genetics
- Clinical Pharmacology and Therapeutics
- Dermatology
- Endocrinology and Diabetes
- Gastroenterology
- Genito-urinary Medicine
- Geriatric Medicine
- Infectious Diseases
- Medical Toxicology
- Medical Oncology
- Pain Medicine
- Palliative Medicine
- Rehabilitation Medicine
- Respiratory Medicine and Pulmonology
- Rheumatology
- Sleep Medicine
- Sports and Exercise Medicine
- Community Medical Services
- Critical Care
- Emergency Medicine
- Forensic Medicine
- Haematology
- History of Medicine
- Browse content in Medical Skills
- Clinical Skills
- Communication Skills
- Nursing Skills
- Surgical Skills
- Browse content in Medical Dentistry
- Oral and Maxillofacial Surgery
- Paediatric Dentistry
- Restorative Dentistry and Orthodontics
- Surgical Dentistry
- Medical Ethics
- Medical Statistics and Methodology
- Browse content in Neurology
- Clinical Neurophysiology
- Neuropathology
- Nursing Studies
- Browse content in Obstetrics and Gynaecology
- Gynaecology
- Occupational Medicine
- Ophthalmology
- Otolaryngology (ENT)
- Browse content in Paediatrics
- Neonatology
- Browse content in Pathology
- Chemical Pathology
- Clinical Cytogenetics and Molecular Genetics
- Histopathology
- Medical Microbiology and Virology
- Patient Education and Information
- Browse content in Pharmacology
- Psychopharmacology
- Browse content in Popular Health
- Caring for Others
- Complementary and Alternative Medicine
- Self-help and Personal Development
- Browse content in Preclinical Medicine
- Cell Biology
- Molecular Biology and Genetics
- Reproduction, Growth and Development
- Primary Care
- Professional Development in Medicine
- Browse content in Psychiatry
- Addiction Medicine
- Child and Adolescent Psychiatry
- Forensic Psychiatry
- Learning Disabilities
- Old Age Psychiatry
- Psychotherapy
- Browse content in Public Health and Epidemiology
- Epidemiology
- Public Health
- Browse content in Radiology
- Clinical Radiology
- Interventional Radiology
- Nuclear Medicine
- Radiation Oncology
- Reproductive Medicine
- Browse content in Surgery
- Cardiothoracic Surgery
- Gastro-intestinal and Colorectal Surgery
- General Surgery
- Neurosurgery
- Paediatric Surgery
- Peri-operative Care
- Plastic and Reconstructive Surgery
- Surgical Oncology
- Transplant Surgery
- Trauma and Orthopaedic Surgery
- Vascular Surgery
- Browse content in Science and Mathematics
- Browse content in Biological Sciences
- Aquatic Biology
- Biochemistry
- Bioinformatics and Computational Biology
- Developmental Biology
- Ecology and Conservation
- Evolutionary Biology
- Genetics and Genomics
- Microbiology
- Molecular and Cell Biology
- Natural History
- Plant Sciences and Forestry
- Research Methods in Life Sciences
- Structural Biology
- Systems Biology
- Zoology and Animal Sciences
- Browse content in Chemistry
- Analytical Chemistry
- Computational Chemistry
- Crystallography
- Environmental Chemistry
- Industrial Chemistry
- Inorganic Chemistry
- Materials Chemistry
- Medicinal Chemistry
- Mineralogy and Gems
- Organic Chemistry
- Physical Chemistry
- Polymer Chemistry
- Study and Communication Skills in Chemistry
- Theoretical Chemistry
- Browse content in Computer Science
- Artificial Intelligence
- Computer Architecture and Logic Design
- Game Studies
- Human-Computer Interaction
- Mathematical Theory of Computation
- Programming Languages
- Software Engineering
- Systems Analysis and Design
- Virtual Reality
- Browse content in Computing
- Business Applications
- Computer Security
- Computer Games
- Computer Networking and Communications
- Digital Lifestyle
- Graphical and Digital Media Applications
- Operating Systems
- Browse content in Earth Sciences and Geography
- Atmospheric Sciences
- Environmental Geography
- Geology and the Lithosphere
- Maps and Map-making
- Meteorology and Climatology
- Oceanography and Hydrology
- Palaeontology
- Physical Geography and Topography
- Regional Geography
- Soil Science
- Urban Geography
- Browse content in Engineering and Technology
- Agriculture and Farming
- Biological Engineering
- Civil Engineering, Surveying, and Building
- Electronics and Communications Engineering
- Energy Technology
- Engineering (General)
- Environmental Science, Engineering, and Technology
- History of Engineering and Technology
- Mechanical Engineering and Materials
- Technology of Industrial Chemistry
- Transport Technology and Trades
- Browse content in Environmental Science
- Applied Ecology (Environmental Science)
- Conservation of the Environment (Environmental Science)
- Environmental Sustainability
- Environmentalist Thought and Ideology (Environmental Science)
- Management of Land and Natural Resources (Environmental Science)
- Natural Disasters (Environmental Science)
- Nuclear Issues (Environmental Science)
- Pollution and Threats to the Environment (Environmental Science)
- Social Impact of Environmental Issues (Environmental Science)
- History of Science and Technology
- Browse content in Materials Science
- Ceramics and Glasses
- Composite Materials
- Metals, Alloying, and Corrosion
- Nanotechnology
- Browse content in Mathematics
- Applied Mathematics
- Biomathematics and Statistics
- History of Mathematics
- Mathematical Education
- Mathematical Finance
- Mathematical Analysis
- Numerical and Computational Mathematics
- Probability and Statistics
- Pure Mathematics
- Browse content in Neuroscience
- Cognition and Behavioural Neuroscience
- Development of the Nervous System
- Disorders of the Nervous System
- History of Neuroscience
- Invertebrate Neurobiology
- Molecular and Cellular Systems
- Neuroendocrinology and Autonomic Nervous System
- Neuroscientific Techniques
- Sensory and Motor Systems
- Browse content in Physics
- Astronomy and Astrophysics
- Atomic, Molecular, and Optical Physics
- Biological and Medical Physics
- Classical Mechanics
- Computational Physics
- Condensed Matter Physics
- Electromagnetism, Optics, and Acoustics
- History of Physics
- Mathematical and Statistical Physics
- Measurement Science
- Nuclear Physics
- Particles and Fields
- Plasma Physics
- Quantum Physics
- Relativity and Gravitation
- Semiconductor and Mesoscopic Physics
- Browse content in Psychology
- Affective Sciences
- Clinical Psychology
- Cognitive Psychology
- Cognitive Neuroscience
- Criminal and Forensic Psychology
- Developmental Psychology
- Educational Psychology
- Evolutionary Psychology
- Health Psychology
- History and Systems in Psychology
- Music Psychology
- Neuropsychology
- Organizational Psychology
- Psychological Assessment and Testing
- Psychology of Human-Technology Interaction
- Psychology Professional Development and Training
- Research Methods in Psychology
- Social Psychology
- Browse content in Social Sciences
- Browse content in Anthropology
- Anthropology of Religion
- Human Evolution
- Medical Anthropology
- Physical Anthropology
- Regional Anthropology
- Social and Cultural Anthropology
- Theory and Practice of Anthropology
- Browse content in Business and Management
- Business Ethics
- Business Strategy
- Business History
- Business and Technology
- Business and Government
- Business and the Environment
- Comparative Management
- Corporate Governance
- Corporate Social Responsibility
- Entrepreneurship
- Health Management
- Human Resource Management
- Industrial and Employment Relations
- Industry Studies
- Information and Communication Technologies
- International Business
- Knowledge Management
- Management and Management Techniques
- Operations Management
- Organizational Theory and Behaviour
- Pensions and Pension Management
- Public and Nonprofit Management
- Strategic Management
- Supply Chain Management
- Browse content in Criminology and Criminal Justice
- Criminal Justice
- Criminology
- Forms of Crime
- International and Comparative Criminology
- Youth Violence and Juvenile Justice
- Development Studies
- Browse content in Economics
- Agricultural, Environmental, and Natural Resource Economics
- Asian Economics
- Behavioural Finance
- Behavioural Economics and Neuroeconomics
- Econometrics and Mathematical Economics
- Economic History
- Economic Systems
- Economic Methodology
- Economic Development and Growth
- Financial Markets
- Financial Institutions and Services
- General Economics and Teaching
- Health, Education, and Welfare
- History of Economic Thought
- International Economics
- Labour and Demographic Economics
- Law and Economics
- Macroeconomics and Monetary Economics
- Microeconomics
- Public Economics
- Urban, Rural, and Regional Economics
- Welfare Economics
- Browse content in Education
- Adult Education and Continuous Learning
- Care and Counselling of Students
- Early Childhood and Elementary Education
- Educational Equipment and Technology
- Educational Strategies and Policy
- Higher and Further Education
- Organization and Management of Education
- Philosophy and Theory of Education
- Schools Studies
- Secondary Education
- Teaching of a Specific Subject
- Teaching of Specific Groups and Special Educational Needs
- Teaching Skills and Techniques
- Browse content in Environment
- Applied Ecology (Social Science)
- Climate Change
- Conservation of the Environment (Social Science)
- Environmentalist Thought and Ideology (Social Science)
- Management of Land and Natural Resources (Social Science)
- Natural Disasters (Environment)
- Social Impact of Environmental Issues (Social Science)
- Sustainability
- Browse content in Human Geography
- Cultural Geography
- Economic Geography
- Political Geography
- Browse content in Interdisciplinary Studies
- Communication Studies
- Museums, Libraries, and Information Sciences
- Browse content in Politics
- African Politics
- Asian Politics
- Chinese Politics
- Comparative Politics
- Conflict Politics
- Elections and Electoral Studies
- Environmental Politics
- Ethnic Politics
- European Union
- Foreign Policy
- Gender and Politics
- Human Rights and Politics
- Indian Politics
- International Relations
- International Organization (Politics)
- International Political Economy
- Irish Politics
- Latin American Politics
- Middle Eastern Politics
- Political Behaviour
- Political Economy
- Political Institutions
- Political Methodology
- Political Communication
- Political Philosophy
- Political Sociology
- Political Theory
- Politics and Law
- Politics of Development
- Public Policy
- Public Administration
- Qualitative Political Methodology
- Quantitative Political Methodology
- Regional Political Studies
- Russian Politics
- Security Studies
- State and Local Government
- UK Politics
- US Politics
- Browse content in Regional and Area Studies
- African Studies
- Asian Studies
- East Asian Studies
- Japanese Studies
- Latin American Studies
- Middle Eastern Studies
- Native American Studies
- Scottish Studies
- Browse content in Research and Information
- Research Methods
- Browse content in Social Work
- Addictions and Substance Misuse
- Adoption and Fostering
- Care of the Elderly
- Child and Adolescent Social Work
- Couple and Family Social Work
- Direct Practice and Clinical Social Work
- Emergency Services
- Human Behaviour and the Social Environment
- International and Global Issues in Social Work
- Mental and Behavioural Health
- Social Justice and Human Rights
- Social Policy and Advocacy
- Social Work and Crime and Justice
- Social Work Macro Practice
- Social Work Practice Settings
- Social Work Research and Evidence-based Practice
- Welfare and Benefit Systems
- Browse content in Sociology
- Childhood Studies
- Community Development
- Comparative and Historical Sociology
- Economic Sociology
- Gender and Sexuality
- Gerontology and Ageing
- Health, Illness, and Medicine
- Marriage and the Family
- Migration Studies
- Occupations, Professions, and Work
- Organizations
- Population and Demography
- Race and Ethnicity
- Social Theory
- Social Movements and Social Change
- Social Research and Statistics
- Social Stratification, Inequality, and Mobility
- Sociology of Religion
- Sociology of Education
- Sport and Leisure
- Urban and Rural Studies
- Browse content in Warfare and Defence
- Defence Strategy, Planning, and Research
- Land Forces and Warfare
- Military Administration
- Military Life and Institutions
- Naval Forces and Warfare
- Other Warfare and Defence Issues
- Peace Studies and Conflict Resolution
- Weapons and Equipment

A newer edition of this book is available.
- < Previous chapter
- Next chapter >
6 SFBT in Action: Case Examples of School Social Workers Using SFBT
Author Webpage
- Published: April 2008
- Cite Icon Cite
- Permissions Icon Permissions
This chapter presents five case studies which show how school social workers adapted solution-focused brief therapy (SFBT) to their school contexts. Using a variety of treatment modalities (family, small group, and macropractice), these school social workers demonstrate how flexible and powerful SFBT ideas can be in a school setting.
Personal account
- Sign in with email/username & password
- Get email alerts
- Save searches
- Purchase content
- Activate your purchase/trial code
- Add your ORCID iD
Institutional access
Sign in with a library card.
- Sign in with username/password
- Recommend to your librarian
- Institutional account management
- Get help with access
Access to content on Oxford Academic is often provided through institutional subscriptions and purchases. If you are a member of an institution with an active account, you may be able to access content in one of the following ways:
IP based access
Typically, access is provided across an institutional network to a range of IP addresses. This authentication occurs automatically, and it is not possible to sign out of an IP authenticated account.
Choose this option to get remote access when outside your institution. Shibboleth/Open Athens technology is used to provide single sign-on between your institution’s website and Oxford Academic.
- Click Sign in through your institution.
- Select your institution from the list provided, which will take you to your institution's website to sign in.
- When on the institution site, please use the credentials provided by your institution. Do not use an Oxford Academic personal account.
- Following successful sign in, you will be returned to Oxford Academic.
If your institution is not listed or you cannot sign in to your institution’s website, please contact your librarian or administrator.
Enter your library card number to sign in. If you cannot sign in, please contact your librarian.
Society Members
Society member access to a journal is achieved in one of the following ways:
Sign in through society site
Many societies offer single sign-on between the society website and Oxford Academic. If you see ‘Sign in through society site’ in the sign in pane within a journal:
- Click Sign in through society site.
- When on the society site, please use the credentials provided by that society. Do not use an Oxford Academic personal account.
If you do not have a society account or have forgotten your username or password, please contact your society.
Sign in using a personal account
Some societies use Oxford Academic personal accounts to provide access to their members. See below.
A personal account can be used to get email alerts, save searches, purchase content, and activate subscriptions.
Some societies use Oxford Academic personal accounts to provide access to their members.
Viewing your signed in accounts
Click the account icon in the top right to:
- View your signed in personal account and access account management features.
- View the institutional accounts that are providing access.
Signed in but can't access content
Oxford Academic is home to a wide variety of products. The institutional subscription may not cover the content that you are trying to access. If you believe you should have access to that content, please contact your librarian.
For librarians and administrators, your personal account also provides access to institutional account management. Here you will find options to view and activate subscriptions, manage institutional settings and access options, access usage statistics, and more.
Our books are available by subscription or purchase to libraries and institutions.
| Month: | Total Views: |
|---|---|
| October 2022 | 4 |
| November 2022 | 1 |
| December 2022 | 2 |
| March 2023 | 5 |
| April 2023 | 4 |
| May 2023 | 1 |
| June 2023 | 3 |
| July 2023 | 4 |
| August 2023 | 2 |
| September 2023 | 2 |
| October 2023 | 2 |
| November 2023 | 2 |
| December 2023 | 6 |
| February 2024 | 1 |
| March 2024 | 5 |
| April 2024 | 3 |
| May 2024 | 5 |
| June 2024 | 1 |
- About Oxford Academic
- Publish journals with us
- University press partners
- What we publish
- New features
- Open access
- Rights and permissions
- Accessibility
- Advertising
- Media enquiries
- Oxford University Press
- Oxford Languages
- University of Oxford
Oxford University Press is a department of the University of Oxford. It furthers the University's objective of excellence in research, scholarship, and education by publishing worldwide
- Copyright © 2024 Oxford University Press
- Cookie settings
- Cookie policy
- Privacy policy
- Legal notice
This Feature Is Available To Subscribers Only
Sign In or Create an Account
This PDF is available to Subscribers Only
For full access to this pdf, sign in to an existing account, or purchase an annual subscription.
Human Subjects Office
Medical terms in lay language.
Please use these descriptions in place of medical jargon in consent documents, recruitment materials and other study documents. Note: These terms are not the only acceptable plain language alternatives for these vocabulary words.
This glossary of terms is derived from a list copyrighted by the University of Kentucky, Office of Research Integrity (1990).
For clinical research-specific definitions, see also the Clinical Research Glossary developed by the Multi-Regional Clinical Trials (MRCT) Center of Brigham and Women’s Hospital and Harvard and the Clinical Data Interchange Standards Consortium (CDISC) .
Alternative Lay Language for Medical Terms for use in Informed Consent Documents
A B C D E F G H I J K L M N O P Q R S T U V W X Y Z
ABDOMEN/ABDOMINAL body cavity below diaphragm that contains stomach, intestines, liver and other organs ABSORB take up fluids, take in ACIDOSIS condition when blood contains more acid than normal ACUITY clearness, keenness, esp. of vision and airways ACUTE new, recent, sudden, urgent ADENOPATHY swollen lymph nodes (glands) ADJUVANT helpful, assisting, aiding, supportive ADJUVANT TREATMENT added treatment (usually to a standard treatment) ANTIBIOTIC drug that kills bacteria and other germs ANTIMICROBIAL drug that kills bacteria and other germs ANTIRETROVIRAL drug that works against the growth of certain viruses ADVERSE EFFECT side effect, bad reaction, unwanted response ALLERGIC REACTION rash, hives, swelling, trouble breathing AMBULATE/AMBULATION/AMBULATORY walk, able to walk ANAPHYLAXIS serious, potentially life-threatening allergic reaction ANEMIA decreased red blood cells; low red cell blood count ANESTHETIC a drug or agent used to decrease the feeling of pain, or eliminate the feeling of pain by putting you to sleep ANGINA pain resulting from not enough blood flowing to the heart ANGINA PECTORIS pain resulting from not enough blood flowing to the heart ANOREXIA disorder in which person will not eat; lack of appetite ANTECUBITAL related to the inner side of the forearm ANTIBODY protein made in the body in response to foreign substance ANTICONVULSANT drug used to prevent seizures ANTILIPEMIC a drug that lowers fat levels in the blood ANTITUSSIVE a drug used to relieve coughing ARRHYTHMIA abnormal heartbeat; any change from the normal heartbeat ASPIRATION fluid entering the lungs, such as after vomiting ASSAY lab test ASSESS to learn about, measure, evaluate, look at ASTHMA lung disease associated with tightening of air passages, making breathing difficult ASYMPTOMATIC without symptoms AXILLA armpit
BENIGN not malignant, without serious consequences BID twice a day BINDING/BOUND carried by, to make stick together, transported BIOAVAILABILITY the extent to which a drug or other substance becomes available to the body BLOOD PROFILE series of blood tests BOLUS a large amount given all at once BONE MASS the amount of calcium and other minerals in a given amount of bone BRADYARRHYTHMIAS slow, irregular heartbeats BRADYCARDIA slow heartbeat BRONCHOSPASM breathing distress caused by narrowing of the airways
CARCINOGENIC cancer-causing CARCINOMA type of cancer CARDIAC related to the heart CARDIOVERSION return to normal heartbeat by electric shock CATHETER a tube for withdrawing or giving fluids CATHETER a tube placed near the spinal cord and used for anesthesia (indwelling epidural) during surgery CENTRAL NERVOUS SYSTEM (CNS) brain and spinal cord CEREBRAL TRAUMA damage to the brain CESSATION stopping CHD coronary heart disease CHEMOTHERAPY treatment of disease, usually cancer, by chemical agents CHRONIC continuing for a long time, ongoing CLINICAL pertaining to medical care CLINICAL TRIAL an experiment involving human subjects COMA unconscious state COMPLETE RESPONSE total disappearance of disease CONGENITAL present before birth CONJUNCTIVITIS redness and irritation of the thin membrane that covers the eye CONSOLIDATION PHASE treatment phase intended to make a remission permanent (follows induction phase) CONTROLLED TRIAL research study in which the experimental treatment or procedure is compared to a standard (control) treatment or procedure COOPERATIVE GROUP association of multiple institutions to perform clinical trials CORONARY related to the blood vessels that supply the heart, or to the heart itself CT SCAN (CAT) computerized series of x-rays (computerized tomography) CULTURE test for infection, or for organisms that could cause infection CUMULATIVE added together from the beginning CUTANEOUS relating to the skin CVA stroke (cerebrovascular accident)
DERMATOLOGIC pertaining to the skin DIASTOLIC lower number in a blood pressure reading DISTAL toward the end, away from the center of the body DIURETIC "water pill" or drug that causes increase in urination DOPPLER device using sound waves to diagnose or test DOUBLE BLIND study in which neither investigators nor subjects know what drug or treatment the subject is receiving DYSFUNCTION state of improper function DYSPLASIA abnormal cells
ECHOCARDIOGRAM sound wave test of the heart EDEMA excess fluid collecting in tissue EEG electric brain wave tracing (electroencephalogram) EFFICACY effectiveness ELECTROCARDIOGRAM electrical tracing of the heartbeat (ECG or EKG) ELECTROLYTE IMBALANCE an imbalance of minerals in the blood EMESIS vomiting EMPIRIC based on experience ENDOSCOPIC EXAMINATION viewing an internal part of the body with a lighted tube ENTERAL by way of the intestines EPIDURAL outside the spinal cord ERADICATE get rid of (such as disease) Page 2 of 7 EVALUATED, ASSESSED examined for a medical condition EXPEDITED REVIEW rapid review of a protocol by the IRB Chair without full committee approval, permitted with certain low-risk research studies EXTERNAL outside the body EXTRAVASATE to leak outside of a planned area, such as out of a blood vessel
FDA U.S. Food and Drug Administration, the branch of federal government that approves new drugs FIBROUS having many fibers, such as scar tissue FIBRILLATION irregular beat of the heart or other muscle
GENERAL ANESTHESIA pain prevention by giving drugs to cause loss of consciousness, as during surgery GESTATIONAL pertaining to pregnancy
HEMATOCRIT amount of red blood cells in the blood HEMATOMA a bruise, a black and blue mark HEMODYNAMIC MEASURING blood flow HEMOLYSIS breakdown in red blood cells HEPARIN LOCK needle placed in the arm with blood thinner to keep the blood from clotting HEPATOMA cancer or tumor of the liver HERITABLE DISEASE can be transmitted to one’s offspring, resulting in damage to future children HISTOPATHOLOGIC pertaining to the disease status of body tissues or cells HOLTER MONITOR a portable machine for recording heart beats HYPERCALCEMIA high blood calcium level HYPERKALEMIA high blood potassium level HYPERNATREMIA high blood sodium level HYPERTENSION high blood pressure HYPOCALCEMIA low blood calcium level HYPOKALEMIA low blood potassium level HYPONATREMIA low blood sodium level HYPOTENSION low blood pressure HYPOXEMIA a decrease of oxygen in the blood HYPOXIA a decrease of oxygen reaching body tissues HYSTERECTOMY surgical removal of the uterus, ovaries (female sex glands), or both uterus and ovaries
IATROGENIC caused by a physician or by treatment IDE investigational device exemption, the license to test an unapproved new medical device IDIOPATHIC of unknown cause IMMUNITY defense against, protection from IMMUNOGLOBIN a protein that makes antibodies IMMUNOSUPPRESSIVE drug which works against the body's immune (protective) response, often used in transplantation and diseases caused by immune system malfunction IMMUNOTHERAPY giving of drugs to help the body's immune (protective) system; usually used to destroy cancer cells IMPAIRED FUNCTION abnormal function IMPLANTED placed in the body IND investigational new drug, the license to test an unapproved new drug INDUCTION PHASE beginning phase or stage of a treatment INDURATION hardening INDWELLING remaining in a given location, such as a catheter INFARCT death of tissue due to lack of blood supply INFECTIOUS DISEASE transmitted from one person to the next INFLAMMATION swelling that is generally painful, red, and warm INFUSION slow injection of a substance into the body, usually into the blood by means of a catheter INGESTION eating; taking by mouth INTERFERON drug which acts against viruses; antiviral agent INTERMITTENT occurring (regularly or irregularly) between two time points; repeatedly stopping, then starting again INTERNAL within the body INTERIOR inside of the body INTRAMUSCULAR into the muscle; within the muscle INTRAPERITONEAL into the abdominal cavity INTRATHECAL into the spinal fluid INTRAVENOUS (IV) through the vein INTRAVESICAL in the bladder INTUBATE the placement of a tube into the airway INVASIVE PROCEDURE puncturing, opening, or cutting the skin INVESTIGATIONAL NEW DRUG (IND) a new drug that has not been approved by the FDA INVESTIGATIONAL METHOD a treatment method which has not been proven to be beneficial or has not been accepted as standard care ISCHEMIA decreased oxygen in a tissue (usually because of decreased blood flow)
LAPAROTOMY surgical procedure in which an incision is made in the abdominal wall to enable a doctor to look at the organs inside LESION wound or injury; a diseased patch of skin LETHARGY sleepiness, tiredness LEUKOPENIA low white blood cell count LIPID fat LIPID CONTENT fat content in the blood LIPID PROFILE (PANEL) fat and cholesterol levels in the blood LOCAL ANESTHESIA creation of insensitivity to pain in a small, local area of the body, usually by injection of numbing drugs LOCALIZED restricted to one area, limited to one area LUMEN the cavity of an organ or tube (e.g., blood vessel) LYMPHANGIOGRAPHY an x-ray of the lymph nodes or tissues after injecting dye into lymph vessels (e.g., in feet) LYMPHOCYTE a type of white blood cell important in immunity (protection) against infection LYMPHOMA a cancer of the lymph nodes (or tissues)
MALAISE a vague feeling of bodily discomfort, feeling badly MALFUNCTION condition in which something is not functioning properly MALIGNANCY cancer or other progressively enlarging and spreading tumor, usually fatal if not successfully treated MEDULLABLASTOMA a type of brain tumor MEGALOBLASTOSIS change in red blood cells METABOLIZE process of breaking down substances in the cells to obtain energy METASTASIS spread of cancer cells from one part of the body to another METRONIDAZOLE drug used to treat infections caused by parasites (invading organisms that take up living in the body) or other causes of anaerobic infection (not requiring oxygen to survive) MI myocardial infarction, heart attack MINIMAL slight MINIMIZE reduce as much as possible Page 4 of 7 MONITOR check on; keep track of; watch carefully MOBILITY ease of movement MORBIDITY undesired result or complication MORTALITY death MOTILITY the ability to move MRI magnetic resonance imaging, diagnostic pictures of the inside of the body, created using magnetic rather than x-ray energy MUCOSA, MUCOUS MEMBRANE moist lining of digestive, respiratory, reproductive, and urinary tracts MYALGIA muscle aches MYOCARDIAL pertaining to the heart muscle MYOCARDIAL INFARCTION heart attack
NASOGASTRIC TUBE placed in the nose, reaching to the stomach NCI the National Cancer Institute NECROSIS death of tissue NEOPLASIA/NEOPLASM tumor, may be benign or malignant NEUROBLASTOMA a cancer of nerve tissue NEUROLOGICAL pertaining to the nervous system NEUTROPENIA decrease in the main part of the white blood cells NIH the National Institutes of Health NONINVASIVE not breaking, cutting, or entering the skin NOSOCOMIAL acquired in the hospital
OCCLUSION closing; blockage; obstruction ONCOLOGY the study of tumors or cancer OPHTHALMIC pertaining to the eye OPTIMAL best, most favorable or desirable ORAL ADMINISTRATION by mouth ORTHOPEDIC pertaining to the bones OSTEOPETROSIS rare bone disorder characterized by dense bone OSTEOPOROSIS softening of the bones OVARIES female sex glands
PARENTERAL given by injection PATENCY condition of being open PATHOGENESIS development of a disease or unhealthy condition PERCUTANEOUS through the skin PERIPHERAL not central PER OS (PO) by mouth PHARMACOKINETICS the study of the way the body absorbs, distributes, and gets rid of a drug PHASE I first phase of study of a new drug in humans to determine action, safety, and proper dosing PHASE II second phase of study of a new drug in humans, intended to gather information about safety and effectiveness of the drug for certain uses PHASE III large-scale studies to confirm and expand information on safety and effectiveness of new drug for certain uses, and to study common side effects PHASE IV studies done after the drug is approved by the FDA, especially to compare it to standard care or to try it for new uses PHLEBITIS irritation or inflammation of the vein PLACEBO an inactive substance; a pill/liquid that contains no medicine PLACEBO EFFECT improvement seen with giving subjects a placebo, though it contains no active drug/treatment PLATELETS small particles in the blood that help with clotting POTENTIAL possible POTENTIATE increase or multiply the effect of a drug or toxin (poison) by giving another drug or toxin at the same time (sometimes an unintentional result) POTENTIATOR an agent that helps another agent work better PRENATAL before birth PROPHYLAXIS a drug given to prevent disease or infection PER OS (PO) by mouth PRN as needed PROGNOSIS outlook, probable outcomes PRONE lying on the stomach PROSPECTIVE STUDY following patients forward in time PROSTHESIS artificial part, most often limbs, such as arms or legs PROTOCOL plan of study PROXIMAL closer to the center of the body, away from the end PULMONARY pertaining to the lungs
QD every day; daily QID four times a day
RADIATION THERAPY x-ray or cobalt treatment RANDOM by chance (like the flip of a coin) RANDOMIZATION chance selection RBC red blood cell RECOMBINANT formation of new combinations of genes RECONSTITUTION putting back together the original parts or elements RECUR happen again REFRACTORY not responding to treatment REGENERATION re-growth of a structure or of lost tissue REGIMEN pattern of giving treatment RELAPSE the return of a disease REMISSION disappearance of evidence of cancer or other disease RENAL pertaining to the kidneys REPLICABLE possible to duplicate RESECT remove or cut out surgically RETROSPECTIVE STUDY looking back over past experience
SARCOMA a type of cancer SEDATIVE a drug to calm or make less anxious SEMINOMA a type of testicular cancer (found in the male sex glands) SEQUENTIALLY in a row, in order SOMNOLENCE sleepiness SPIROMETER an instrument to measure the amount of air taken into and exhaled from the lungs STAGING an evaluation of the extent of the disease STANDARD OF CARE a treatment plan that the majority of the medical community would accept as appropriate STENOSIS narrowing of a duct, tube, or one of the blood vessels in the heart STOMATITIS mouth sores, inflammation of the mouth STRATIFY arrange in groups for analysis of results (e.g., stratify by age, sex, etc.) STUPOR stunned state in which it is difficult to get a response or the attention of the subject SUBCLAVIAN under the collarbone SUBCUTANEOUS under the skin SUPINE lying on the back SUPPORTIVE CARE general medical care aimed at symptoms, not intended to improve or cure underlying disease SYMPTOMATIC having symptoms SYNDROME a condition characterized by a set of symptoms SYSTOLIC top number in blood pressure; pressure during active contraction of the heart
TERATOGENIC capable of causing malformations in a fetus (developing baby still inside the mother’s body) TESTES/TESTICLES male sex glands THROMBOSIS clotting THROMBUS blood clot TID three times a day TITRATION a method for deciding on the strength of a drug or solution; gradually increasing the dose T-LYMPHOCYTES type of white blood cells TOPICAL on the surface TOPICAL ANESTHETIC applied to a certain area of the skin and reducing pain only in the area to which applied TOXICITY side effects or undesirable effects of a drug or treatment TRANSDERMAL through the skin TRANSIENTLY temporarily TRAUMA injury; wound TREADMILL walking machine used to test heart function
UPTAKE absorbing and taking in of a substance by living tissue
VALVULOPLASTY plastic repair of a valve, especially a heart valve VARICES enlarged veins VASOSPASM narrowing of the blood vessels VECTOR a carrier that can transmit disease-causing microorganisms (germs and viruses) VENIPUNCTURE needle stick, blood draw, entering the skin with a needle VERTICAL TRANSMISSION spread of disease
WBC white blood cell

COMMENTS
Empowering a Survivor of Domestic Violence - Social Work Case Study Examples and Answers. Introduction: This social work case study examples and answers scenario centers on Jane, a 33-year-old woman who has recently escaped an abusive relationship. She has two young children and seeks support in rebuilding her life and ensuring her safety.
Grand Challenges Faculty Development Institute: Eradicate Social Isolation CSWE, Dallas, TX, Oct. 19, 2017 1 Case Studies The following case studies were included to highlight different ways that social workers can assess and intervene with issues of social isolation. These cases are free to you to use, modify, and incorporate into your teaching.
Case Vignette 3: Middle Childhood. Monty is an 8-year-old boy living with his mother, Foley, and maternal grandmother, Livia, in a small 2-bedroom apartment in the city. Foley was 15 when she had Monty and did not finish high school. Both she and her mother Livia work different shifts at a factory nearby their apartment so one of them can be ...
Real Cases Project: The Anne M. Case Study 1 Integrating Child Welfare Practice Across the Social Work Curriculum Real Cases Project: The Case Studies ANNE M. CASE STUDY Case Details Borough: Bronx Type of Report: Initial Source of Report: Social worker, Douglas Hospital Date of Intake: 7/16/07 ...
Case Study 2: Josef. Summary. Download the whole case study as a PDF file. Josef is 16 and lives with his mother, Dorota, who was diagnosed with Bipolar disorder seven years ago. Josef was born in England. His parents are Polish and his father sees him infrequently. This case study looks at the impact of caring for someone with a mental health ...
Identify a case(s) for student to read and review. Provide specific prompts that you would like the student to address as a part of the assignment. Include prompts that have the student address the case from a clinical and macro viewpoint as well as consider some ethical considerations.
This is a social development case study of a student who has been relying his education on scholarship. Unfortunately, challenges had been haunting him ever since he was young. Nevertheless, he ...
The three case studies collectively raise critical issues in public child welfare practice today, show a diverse range of practices, family issues, and populations, as well as showcase the ChildStat Initiative. The Real Cases Project is part of the social work tradition of case study education. During our profession's history, social work ...
Practising Social Work Research: Case Studies for Learning, second edition (ToC) May 2017. Publisher: University of Toronto Press. Authors: Rick Csiernik. King's University College. Rachel ...
This paper describes a novel approach which taught practice research and introduced a range of class and field activities in a 2-semester social work research courses, including case studies ...
Oranga Tamariki (2022b) provide an example of a good and poor case note. Social Work Haven (2021) has developed a case notes cheat sheet. Sommers-Flanagan (2009) provide a detailed intake report template.
Case study research is a good fit with many forms of social work. practice. Although disparaged as uncontrolled and uninterpretable, the case study has great potential for building social work knowledge for assessment, intervention, and outcome. This article defines case study research, presents guidelines for evaluating case studies, and shows ...
Social work report: Background. Mrs Beryl Brown (01/11/33) is an 85 year old woman who was admitted to the Hume Hospital by ambulance after being found by her youngest daughter lying in front of her toilet. Her daughter estimates that she may have been on the ground overnight. On admission, Mrs Brown was diagnosed with a right sided stroke ...
Abstract. Case study research is a good fit with many forms of social work practice. Although disparaged as uncontrolled and uninterpretable, the case study has great potential for building social work knowledge for assessment, intervention, and outcome. This article defines case study research, presents guidelines for evaluating case studies ...
social work case study sample - Free download as Word Doc (.doc / .docx), PDF File (.pdf), Text File (.txt) or read online for free. This social case study report summarizes information about Pastora C. Cabando, a 55-year-old married woman from Kolambugan, Lanao del Norte who has been suffering from dengue fever for 3 weeks. The report details her family composition, medical history and ...
social-work-case-study-examples - Free download as PDF File (.pdf), Text File (.txt) or read online for free.
The main concern in evaluating a case study is to accurately assess its quality and ultimately to offer clients social work interventions informed by the best available evidence. To assess the ...
Example 1. 04/04/2021 at 10:30am. (this is the time the call/visit took place) Home visit to Beth to discuss children's poor school attendance. Beth expressed having no transport for children to attend school since her car broke down. Beth said she was feeling low and would like to engage in some social activities.
Executive Order Hapag 2023. EJ1308731 - Yutx. WORK Immersion Portfolio. Project-Proposal-sample. Case Studies, General Intake, Project Proposal (Individual, Family and Group) This is a sample activity of an Individual Case Study in which the student chose a client to be interviewed and then base her study on the response and.
In the case study example that follows, one school social worker we worked with described a case where she saw a family of a student at her school for a six-session SFBT course of treatment. Carol (name changed for confidentiality)is a school social worker in the large suburban district of Forest Side, outside of Chicago.
BACHELOR OF SCIENCE IN SOCIAL WORK. Course: Bachelor of Science in Social Work S. Y. 2nd Sem. Subject: SW 113 Social Work Practice with Individuals and Families 2021 - 2022. SOCIAL CASE STUDY REPORT. Date of meeting: May 25, 2022: Wednesday. Client's full name: Amandita S. Sabangan. Age: 47 Birth order: First Born Sex/Gender: Female Status ...
In the case study, the researcher is interested in the case and aims at its in-depth investigation (Bryman, 2016). Gilgun (1994) argues that a case study can be an effective method in social work ...
Example Of Case Study In Social Work. Satisfactory Essays. 160 Words. 1 Page. Open Document. Precious is a 17-year-old who is dealing with PTSD. Client has been physically, verbally, emotional, and sexually abuse from her mother. Client also was raped by her father and has two children by her father. Client also is diagnosed with HIV/AIDs which ...
Human Subjects Office / IRB Hardin Library, Suite 105A 600 Newton Rd Iowa City, IA 52242-1098. Voice: 319-335-6564 Fax: 319-335-7310